Feds tell states it’s all or nothing on Medicaid expansion; Washington Post map shows Ky. is only state ‘leaning’ toward it
Kentucky Health News
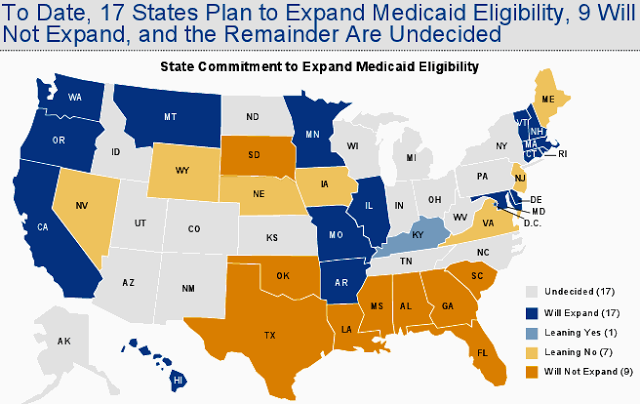
When the Supreme Court upheld federal health reform but said states could opt out of the expansion of Medicaid to people with incomes above the poverty line, to be funded with generous federal subsidies, one of the first questions was whether a state had to go all the way: to 133 percent of poverty (138 percent with an official fudge factor). Now the Obama administration has answered “no.” And that could make the decision tougher for Kentucky, which is the only state The Washington Post listed this month as leaning toward expansion.
The Post’s Sarah Kliff wrote, “The administration’s reasoning goes like this: The federal government
was giving states a really, really good deal on the Medicaid expansion.
It was footing the entire bill for the newly eligible enrollees for
three years,” 2014 through 2016, rather than the 72 percent it pays Kentucky for current enrollees. The subsidy for the new eligibles would drop to 95 percent in 2017, 94 percent in 2018, 93 percent in 2019; and 90 percent in 2020.
White House aides told Kliff that in passing the bill, Congress (which is to say the Democrats in Congress) “gave states that really high
funding in the service of a very specific goal: Ensuring all Americans
have access to insurance options.” But “If a state decided to cover, say, everyone up to the federal poverty line, they would be working with a smaller, more manageable population,” Kliff explains. “Those living above the poverty line, meanwhile, wouldn’t be left in the lurch. The Affordable Care Act allows them to receive very generous subsidies in the private insurance market.”
However, Medicaid Administrator Cindy Mann told Kliff that if states could fall short of the 133 percent level, they wouldn’t be within the spirit of the law. Kliff paraphrases Mann: “They wouldn’t offer
all their residents a way to purchase affordable coverage, and if
they’re not going to do that, the White House says they don’t deserve the
extra funding.”
Gov. Steve Beshear said again today that Kentucky should expand Medicaid “if we can afford it” because so many people in the state have no health insurance and are in poor health, and improving their health would be good for the state’s economy.
Kentucky now makes Medicaid available to people with household incomes below 70 percent of the poverty line, which varies by household size. The Urban Institute has estimated that expanding the program to 133 percent of poverty would cost the state about 5 percent more than it would otherwise spend through 2022. That would be $1.3 billion extra in 2017-22, and some Republicans in the legislature have said the state can’t afford it. The state expects to spend $1.5 billion on Medicaid in the 2013-14 fiscal year.
While the Post lists Kentucky as the only state “leaning yes” to expansion, it seems likely to be joined by several others. “States have stayed mum on whether they will participate in the
expansion, seeing first if they could get a better deal — the partial
expansion,” Kliff writes. “The federal government took a while to show its cards; it
wanted to see if states would sign up for the full expansion, without
giving them a scaled-back option.” Only 17 states have said yes, and as many are undecided, the Post reports.
In setting a firm rule, the White House may think states “will decide the 100
percent match is too good to pass up and that the federal money will
pull everyone in,” Kliff writes. “Or, it could indicate the Obama administration is okay with not all
states participating with the Medicaid expansion on day one. Again, this
wouldn’t be unprecedented: Only six states initially signed up for
Medicaid when it launched in 1965.”
States should realize that expanding Medicaid is a long-term investment in the health of their people that will pay off in the long run, Dr. Wayne Myers, who once ran Kentucky’s rural-health office and was the first director of the federal Office of Rural Health Policy, writes in the Daily Yonder. He says that if a state doesn’t expand Medicaid, many of its people will remain or become uninsured.
“Medicaid is a rural issue because a higher percentage of low-income people live in rural communities, and rural families are less likely to have private health insurance,” Myers writes, adding that the program is also “a major economic driver.” According to the National Center for Rural Health Works at Oklahoma State University, Medicaid was responsible for 113,000 jobs and a total of $10.5 billion in economic activity in Oklahoma in 2010.
Myers cites studies showing that patients with insurance who are hospitalized after accidents are 40 percent less likely to die than those without insurance, because uninsured patients got less attention from medical staff. Opting out of the expansion “may get a governor a self-inflicted gunshot wound to the foot, some dead hospitals and a bunch of dead citizens who needn’t have died,” Myers writes.
Kentucky Health News is a service of the Institute for
Rural Journalism and Community Issues at the University of Kentucky, with
support from the Foundation for a Healthy Kentucky.
