Flexibility Act would give states more Medicaid authority, but it could mean that fewer children would have health coverage
 |
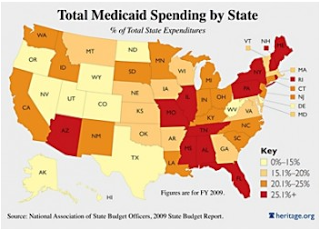
| MEDICAID PERCENTAGE OF TOTAL STATE SPENDING |
Children’s advocates are concerned the proposed State Flexibility Act would result in more children living without health insurance in Kentucky.
The act “would repeal protections put in place for states to maintain current eligibility and enrollment requirements for Medicaid and the Children’s Health Insurance Program, known in Kentucky as K-CHIP,” Renee Shaw of the Public News Service reports.
The goal of the act, its sponsors say, is to give states more flexibility so they can balance their own budgets. “The onerous federal mandates on states today make it especially challenging for states to solve the unprecedented budget crises, and governors have asked Washington for relief from these excessive constraints,” the act reads. In Kentucky, there is a a projected budget shortfall of $780 million for Fiscal 2012, $166.5 million of which is due to a gap in Medicaid funding.
But Lacey McNary, deputy director of Kentucky Youth Advocates, say the move would only further burden families. “Children who in Kentucky are up to 200 percent of the poverty level can enroll, and they’re eligible for K-CHIP,” she said. “In order to save some money, the state could say, ‘We’re only going to cover kids up to 150 percent of poverty’ — thus, covering less children and saving money.”
Estimates show almost half of Kentucky’s children have government-supported health insurance. About 60,000 kids are enrolled in K-CHIP every month and another 386,000 Kentuckians are enrolled in Medicaid, which serves low-income and disabled Americans, including children. “It’s been proven that K-CHIP is a very successful program to get kids covered,” McNary said. “This bill is a permission slip for governors to reduce coverage for kids, to balance the budget.”
If the bill passes, about 14 million children nationwide could be at risk for losing their health insurance, Shaw reports. (Read more)