Ky. is already short of doctors, dentists; how will its health-care system handle expansion of Medicaid and private insurance?
Kentucky Health News
In the wake of Gov. Steve Beshear’s recent decision to expand Medicaid under federal health reform, there is concern that Kentucky’s health-care system will not be able to care for the newly insured.
Health reform means that an estimated 308,000 new Kentuckians will qualify for Medicaid, and 332,000 more will qualify for subsidies to buy private insurance through the state insurance exchange that will start taking enrollments Oct. 1.
But Kentucky already has a health care provider shortage, especially in rural areas. A study for the state estimates that it needs 3,790 more doctors just to meet current demand, to say nothing of what will be needed to care for those who haven’t been a regular part of the health-care system, reports Laura Ungar of The Courier-Journal.
The report by Deloitte Consulting made 11 recommendations, including authority for nurse
practitioners to prescribe less risky drugs without a written
agreement with a doctor, and one that would be even more controversial, putting limits on medical malpractice awards, said Ungar.
The report also recommended expanding and increasing Medicaid reimbursements in rural areas, to encourage more physicians to take Medicaid patients.
It did not mention complaints by health-care providers about getting paid by the managed-care Medicaid system that the state began in November 2011; Gov. Steve Beshear said when he announced Medicaid expansion that those problems are being worked out.
“Consultants
said 61 percent of the 3,790 ‘full-time equivalent’ physicians needed
(which includes primary care doctors and specialists) were in rural
counties,” reports Ungar. Jonathan Felix of Deloitte said, “Primary care, dental care and behavioral health are all big needs in the state.”
The report said the state needed 183 more primary-care doctors, even before Medicaid expansion, but a 2012 Kentucky Physician Workforce Needs Assessment report by the University of Kentucky said the state needs 557 more primary-care physicians and 1,655 more total physicians to meet the national ratios for physicians to population.
The consultants said the state already needs 612 more dentists. It now has 1,711.
Complicated provider shortage problem, no easy answer
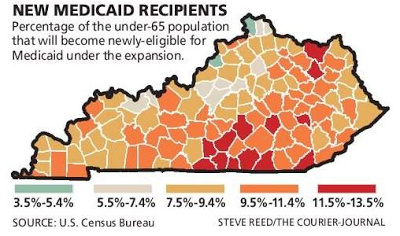
About 192 federally identified areas in Kentucky — including 47 counties — have shortages of health professionals, Ungar reports. Kentucky counties who will have the most non-elderly residents eligible for
Medicaid often have fewer primary-care doctors per person, according to data analyzed by The Courier-Journal. Ungar notes that Casey County, for example, ranks in the bottom third for doctors per capita, but it has the highest portion of newly eligible residents at 13.5 percent.
“We can’t grow physicians fast enough to meet the need, in the rural areas especially,” Susan Zepeda, president and chief executive officer for the Foundation for a Healthy Kentucky, told Ungar.
Nationally, there is a primary-care shortage, partly because such doctors make less money than most, and low reimbursement rates exacerbate that. A 2012 study in the journal Health Affairs said 21 percent of
office-based physicians in Kentucky did not accept new Medicaid patients in 2011, Ungar notes.
The health reform law will raise the Medicaid fees to match what
Medicare pays primary-care doctors, but only for two years. Kentucky’s Medicare rates are about 72 percent of the Medicare rates, compared to a national average of 59 percent, says an Urban Institute study. But the time limit leaves some practitioners wary.
“If I choose to increase the number of Medicaid patients, and two years
down the road that payment drops back to two-thirds, all of a sudden I’m
going to have an awful lot of trouble keeping my doors open,” Reid
Blackwelder, a family practitioner and incoming president of
the American Academy of Family Physicians, told Michael Ollove of Stateline.
A report last year by the non-partisan Center for Studying Health System Change
said the temporary nature of the pay raise could limit its
effectiveness, particularly in Kentucky and other states that are expecting the largest percentage increases in Medicaid enrollees and that have low numbers of primary-care physicians.
“I’m not sure who’s going to pick up all those patients into their practices,” Julianne Ewen, a nurse practitioner in Lexington and president of the Kentucky Coalition of Nurse Practitioners and Nurse Midwives, told Ungar. Legislation to let nurse practitioners prescribe non-scheduled drugs without a doctor agreement failed in the state Senate this year.
While some policy analysts have touted nurse practitioners as a solution to the rural primary-care shortage because they often provide primary care in rural and isolated areas that do not have doctors nearby, they would not be covered by the two-year reimbursement increase. Ewen said the reimbursement is only $23 for a lower-level visit by an established patient.
A possible long-term solution includes greater reliance on community health centers, some say.
And hospital officials said they plan to continue expanding primary care and employ telemedicine. Ruth Brinkley, president and chief
executive officer of KentuckyOne Health, said her system is looking to open new primary care offices and hire more
staff.
Dr. David Dunn, vice president for health affairs at the University of Louisville, said the university is increasing physician training in such areas as family medicine and geriatrics and using funds from its new partner, KentuckyOne, to expand the nursing work force with professionals, such as advanced nurse practitioners.
Health providers and advocates agree that getting more people insured should produce a healthier population in the end. But they
said much remains unknown, including how many of those eligible for coverage under health reform will sign up for it. The state estimates that 188,000 of the 308,000 newly eligible will enroll, but some think that estimate is low.

