Living in a community with high income inequality is bad for your health, study says, and much of Ky. is high in inequality
A study by researchers at the University of Wisconsin for the Robert Wood Johnson Foundation found that not only factors such as smoking and crime rate but also income inequality influenced lifespan, Margot Sanger-Katz writes for The New York Times.
 |
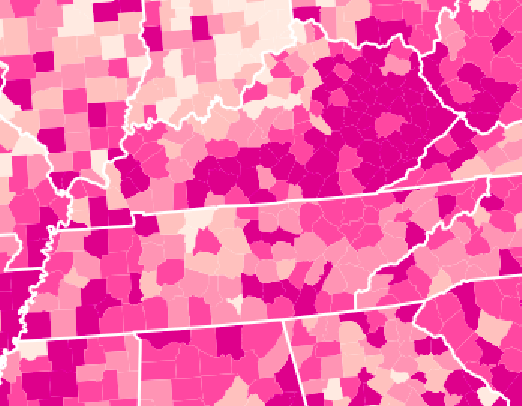
| This close-up of a New York Times graphic shows income inequality in Kentucky, Tennessee and parts of surrounding states. Lighter areas have less inequality, and darker areas have more inequality. |
“It’s not just the level of income in a community that matters—it’s also how income is distributed,” said Bridget Catlin, the co-director of the County Health Rankings and Roadmap project. “The effect of inequality was statistically significant, equivalent to a difference of about 11 days of life between high- and low-inequality places,” Sanger-Katz reports. “The differences were small, but for every increment that a community became more unequal, the proportion of residents dying before the age of 75 went up.”
Other research shows that income inequality affects life expectancies of citizens in countries around the world. Why exactly this happens is debatable. One idea is that though money buys better health, “It makes a bigger difference for people low on the income scale than those at the top,” Sanger-Katz writes. That means a having very few poor individuals in an area will improve average health more than having very few rich individuals will reduce it.
Another theory is that areas where wealthy individuals can “buy their way out of social services may have less cohesion and investment in things like education and public health that we know affect life span,” Sanger-Katz writes. Also, some research indicates that living around richer people is stressful, causing mental health problems or cardiac disease.
To measure inequality, the researchers compared incomes of individuals living in a certain area who earned the 80th percentile with the incomes of those who earned the 20th percentile. They recorded all those who died before age 75 and the age at which they died, calculating “potential life years lost.” A person who died at 70 would have lost five years of potential life.
“For every one-point increase in the ratio between high and low earners in a county, there were about five years lost for every 1,000 people,” Sanger-Katz writes. “That’s about the same difference they observed when a community’s smoking rate increased by 4 percent or its obesity rate rose by 3 percent.”
Through the Patient Protection and Affordable Care Act, Americans at the lower end of the income spectrum are receiving health insurance, at least in states like Kentucky that have expanded Medicaid eligibility, and researchers will track whether those provisions will reduce the effects of inequality in the coming years. (Read more)