Seniors get a lot of anti-anxiety drugs, sometimes in dangerous combination with narcotics; Ky. ranks third in the nation in that
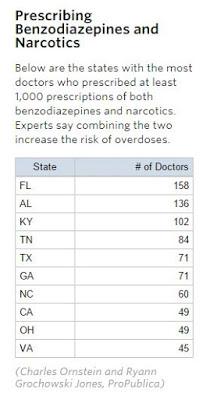

Using anti-anxiety drugs in combination with narcotics increases the risk of overdoses, but Kentucky has many doctors who prescribe a lot of both. More than 100 Kentucky doctors each wrote at least 1,000 prescriptions for both types of drugs in 2013, according to data compiled by ProPublica.
That ranked Kentucky third in the nation, trailing only Florida and Alabama. Other southeastern states dominated the top 10. California, the nation’s most populous state, ranked eighth; Tennessee was fourth and Ohio was ninth.
ProPublica has an application that lets you look up, by doctors’ names, cities or ZIP codes, the number of Medicare claims they filed in 2013, the amount of money, the number of patients and the number of prescriptions for brand-name drugs.
The anti-anxiety drugs, some known as benzodiazepines, include popular tranquilizers such as Valium, Xanax and Ativan.
Lawmakers initially chose to keep them out of Medicare Part D because they had been linked to abuse and an increased risk of falls among the elderly. Doctors kept prescribing them to Medicare enrollees, who found other ways to pay for them.
In 2013, the year Medicare started covering benzodiazepines, it paid for nearly 40 million prescriptions, ProPublica found. Generic versions of Xanax (alprazolam), Ativan (lorazepam) and Klonopin (clonazepam) were among the top 32 most-prescribed medications in Medicare Part D that year.
The American Geriatrics Society “discourages the use of benzodiazepines in seniors for agitation, insomnia or delirium because they can be habit-forming and disorienting and their effects last longer in older patients.” The society does say the drugs “are appropriate to treat seizure disorders, severe anxiety, withdrawal and in end-of-life care,” ProPublica notes.
One geriatric psychiatrist told ProPublica that the drugs are a “very real safety concern” for the elderly, and that he and others in his field don’t use them as a “first-, second-, or third- line of treatment.” Some geriatric psychiatrists have voiced concerns that these drugs are now being used instead of antipsychotics, since Medicare has pushed to reduce the use of antipsychotics, particularly in nursing homes, because of their risks.
Several doctors who rank among Medicare’s top prescribers of the drugs told ProPublica that any risks of anti-anxiety drugs are outweighed by their benefits. One said that the drugs worked well for his patients, many of whom were trying to kick addictions to narcotics, but struggled with anxiety and depression.
However, ProPublica also found that some doctors appear to be prescribing benzodiazepines and narcotic painkillers to the same patients, which increased the risk of misuse and overdose. That’s where Kentucky ranked third.
Dr. Leonard J. Paulozzi, a medical epidemiologist at the federal Centers for Disease Control and Prevention, co-authored an analysis showing that benzodiazepines were involved in about 30 percent of the fatal narcotic overdoses that occurred nationwide in 2010, ProPublica reports.