More Kentucky patients are recuperating in their local, rural hospitals after surgery in an urban hospital
Kentucky Health News
Rural residents are increasingly being transferred out of big urban hospitals to recuperate in rural hospitals, many of which are struggling financially and can use the business.
“We have seen trends of this around the state,” said Elizabeth Cobb, vice president of health policy for the Kentucky Hospital Association, said in an interview.
Oregon’s legislature voted recently to encourage the trend in that state, by appropriating $10 million for rural health-care improvements, with the largest part encouraging such transfers.
In Kentucky, Cobb said the transfers would have to make sense from procedural, convenience and financial perspectives, but when it works out it is great for both the urban and rural hospitals, and also for the families.
“Certainly when there is a treatment or procedure that will take a significant amount of recovery, it is a wonderful thing for rural Kentuckians to be able to transfer back to their community facility to finish off their recuperation,” she said.
Oregon’s program aims to create a more consistent patient population in its rural hospitals, which will help stabilize their funding. At the same time, the program will relieve pressure on strained urban hospitals, Chris Gray reports for The Lund Report.
Rural hospitals are struggling financially all over the country and often have inconsistent patient volumes, while urban hospitals struggle with reaching capacity, and often worry they might have to expand, Gray notes.
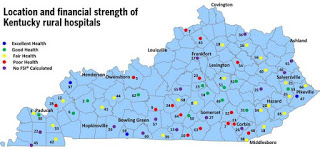
A state report by then-Auditor Adam Edelen last year found that one in three of Kentucky’s rural hospitals were in poor financial condition and suggested that to survive, they might have to adapt to new business models, such as merging with larger hospitals or hiring them as managers, forming coalitions with other hospitals, or finding a health-care niche that hasn’t been served, such as creating a partnership with urban hospitals to allow rural patients the ability to recuperate closer to home.
While it sounds like a “common-sense system,” Gray reports that the program is costly to set up, between $4 and $7 million, but once it is up and running, and the hospitals learn how to coordinate, “it should be self-sustaining, since money from insurers, Medicaid and Medicare will follow the patient,” according to an interim workgroup of rural health officials from Oregon.
A rural health physician told Gray that “local hospitals and healthcare access, along with good public schools, provide the backbone for a viable community when employers are looking to invest in a community,” he writes.
