Kentucky’s uninsured rate drops to 6 percent; states that expanded Medicaid, like Kentucky, saw the greatest drops
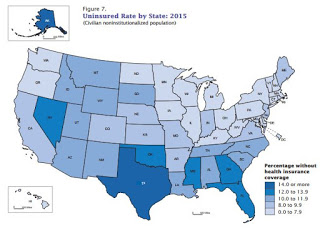
 |
| U.S. Census Bureau map, based on American Community Survey |
The drop reflects a net gain of 355,000 people with insurance, according to the American Community Survey, a continuous poll of the U.S. population. The survey showed an even larger drop among Kentucky children, from 16.6 percent uninsured in 2013 to 4.2 percent in 2015.
Data from 2013 provide a benchmark for comparison because it was the last year before implementation of the Patient Protection and Affordable Care Act, including the expansion of Medicaid in Kentucky to those who earn up to 138 percent of the federal poverty level.
The report found that the 32 states that expanded Medicaid had the largest increases in insurance coverage. Kentucky’s decrease in uninsured appeared to be larger than any other state but California.
Advocacy groups credited the expansion for the decrease, and asked Gov. Matt Bevin to consider that when it comes time to negotiate with the Centers for Medicare and Medicaid Services about the governor’s new plan for Medicaid. The plan is designed to encourage higher levels of participant involvement through premiums and “community engagement” requirements, conditions that could be denied.
Bevin has said he would negotiate with the federal officials, but his plan says it constitutes the conditions under which Kentucky will continue the expansion. A failure of negotiations could take health insurance away from more than 430,000 Kentuckians who now have health insurance through the expansion.
 |
|
Kentucky Center for Economic Policy
|
In its statement, The Kentucky Center for Economic Policy touted the many health and economic benefits that have resulted from the expansion, such as increased preventive care, fewer emergency room visits and reports of improved personal health, and said the current Medicaid proposal creates “barriers to coverage like premiums, lockouts and work requirements that would reduce the number of Kentuckians covered.”
“Because Kentucky has seen the greatest gains, we also have the most to lose if harmful changes to Medicaid are approved,” KCEP Executive Director Jason Bailey said. “Our hope is that the Bevin administration will negotiate in earnest with the federal government to find a way to build on our successes and not move backward on our health progress.”
Kentucky Youth Advocates noted that eligibility for children in Medicaid and the Kentucky Children’s Health Insurance Program did not change from 2013-15, “indicating that the increases in coverage for children were likely an indirect result of more parents gaining health insurance through Medicaid expansion.”
“We know that when parents have health insurance, their children are more likely to have health insurance,” Dr. Terry Brooks, executive director of KYA, said in a statement. “We encourage Gov. Bevin to negotiate with CMS on a Medicaid proposal that continues affordable coverage for families and does not result in people losing coverage.”
Bevin spokeswoman Amanda Stamper also noted that most of the new enrollment came from the expansion of Medicaid, and painted a different picture of this reality. “This is a sad commentary on the economic state of Kentucky and is not sustainable,” Stamper told John Cheves of the Lexington Herald-Leader. “While some are focused solely on enrollment, Gov. Bevin is focused on driving better health and employment outcomes and the long-term fiscal sustainability of the Medicaid program.”
Bevin’s proposal says it “is expected to save taxpayers $2.2 billion over the five-year waiver period,” by reducing enrollment in the program by about 88,000 people in the next five years, but only $331 million of that would be state tax money, because the federal government covers the bulk of Medicaid costs.