Study finds Kentucky hospitals had 77% less charity care in first two years of Obamacare; ER visits were about the same
“Thousands more Kentuckians had insurance in 2015 than in 2012, and that led to a huge drop in the value of the charity care hospitals provided,” Ben Chandler, president and CEO of the Foundation for a Healthy Kentucky, said in a news release. “Charity care and uncollected bills comprise a significant portion of uncompensated care provided by Kentucky hospitals, and hospitals in other states that, like Kentucky, have expanded Medicaid also have seen large decreases in the charity care.”
The Foundation for a Healthy Kentucky is paying the State Health Access Data Assistance Center at the University of Minnesota more than $280,000 over a three-year period to study the impact of the Patient Protection and Affordable Care Act in Kentucky.
 |
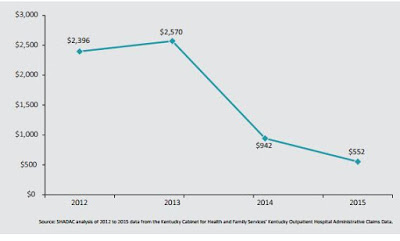
| Hospital Charity Care and Self-Pay Charges in Dollars (millions), Kentucky, 2012-2015 |
In 2013, prior to implementation of the reform law and the state’s expansion of Medicaid to those who earn up to 138 percent of the federal poverty level, Kentucky hospitals provided nearly $2.6 billion dollars in uncompensated care. This dropped to $942 million in 2014, and to $522 million in 2015.
Kentucky hospitals provided almost 77 percent less charity care and care to the uninsured for Kentuckians in 2015 than they did in 2012 suggesting that Kentucky hospitals are now being paid for a larger percentage of care they provide to low-income patients who previously were uninsured, says the release.
The study also looked at potentially avoidable hospital admissions and usage of emergency departments.
It found that hospitals saw a decrease in admissions for two chronic conditions, high-blood pressure and asthma, but saw an increase in admissions for diabetes.
The report also found that nearly 25 percent of Kentuckians used an emergency department in 2014, a decrease from 30.4 percent in 2012.
Kentucky’s rate for emergency-department use is significantly higher than the national average of 18.2 percent. It is higher than two neighboring states, Missouri and Virginia, and about the same as Arkansas, Illinois, Indiana, Ohio, West Virginia, and Tennessee.
 |
| ED visits in the past year by age, Kentucky, 2012-2014 |
About 29 percent of those who used the emergency department said it was because of a medical emergency; almost 29 percent said they did so because other facilities weren’t open when they needed care; and 18 percent only named a specific health condition. Seven percent said they were following a doctor’s order, 3 percent said they were nearby, and 3 percent said they were taken there by first responders. Eight percent gave other answers.
Elderly Kentuckians continued to report the highest rate of emergency visits at 32 percent, and were the age group with the least decline from 2012 to 2014.
People 65 and over are on Medicare. The report found that more people on public insurance plans used the emergency department than did people on private plans, 48 percent and 19 percent respectively.
“ED utilization reflects the greater health needs of the surrounding community and may provide the only readily available care for individuals who cannot obtain care elsewhere,” the report says. “Many ED visits are ‘resource sensitive’ and potentially preventable, meaning that access to high-quality, community-based health care can prevent the need for a portion of ED visits.”
This semi-annual report also analyzed data regarding health coverage, access to care, cost of care, quality of care and health outcomes and included the results of a spring 2016 Kentucky Health Reform Survey of non-elderly Kentucky adults. Click here for a copy of the report.