UK center promotes at-home test for colorectal cancer, reports on efforts to get young women vaccinated for cervical cancer
In July 2014, the center received a $3.75 million, five-year grant renewal from the federal Centers for Disease Control and Prevention for a colorectal cancer at-home screening prevention project in Central Appalachia and other rural areas. The UK Center is one of 26 CDC-funded Prevention Research Centers in the country.
Tom Collins, associate director of the RCPC, gave an update on its project at a Center for Clinical and Translational Science clinical research update meeting at UK Oct.18. Robin Vanderpool, associate professor in the College of Public Health, discussed the results and successes of its completed cervical-cancer screening project.
Early screening and prevention are key to surviving colorectal cancer. The CDC says that most deaths caused by colorectal cancer could be prevented if everyone over the age of 50 got screened. And if detected early, treatment for colorectal cancer is highly effective.
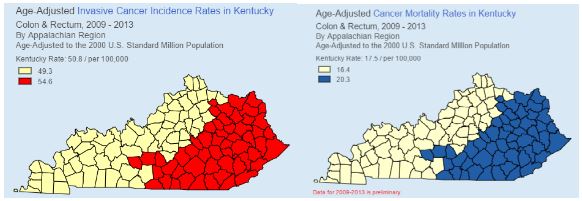
In 2013, the last year for which data is available, Kentucky ranked first in colon cancer and fourth in colon-cancer deaths, according to the Colon Cancer Prevention Project.
The project’s title and motto is “I did FIT.” FIT stands for fecal immunochemical test, an at-home test that allows a person to collect a small stool sample in the privacy of their home and mail it in a provided kit to the lab for testing. The FIT test must be done every year.
Since June 2015, the UK center has distributed more than 700 kits, with a 60 percent return rate in the eight-county Kentucky River Health District. Those with a positive test result, about one in six, have been offered a colonoscopy with follow-up; the rest have been invited to be part of the research, which is ongoing.
To help determine the best way to get people to do a yearly test, researchers divided the volunteer participants into two groups: one that gets social media and personal messages about it along with the traditional standard of care and another that gets standard of care alone. A year and a half remains in this portion of the research.
Cervical cancer and the HPV vaccine
Collins said they are trying to build on the success of the UK Center’s previous prevention program for cervical cancer prevention and screening, called “1-2-3 Pap.”
 |
| Prevention Research Center graphic; click on it to view a larger version |
This UK center study promoted the human papillomavirus vaccination to prevent cervical cancer in Appalachia, which also has a higher incidence and mortality rate for cervical cancer than the rest of the state.
The three-dose HPV vaccine was approved by the federal government 10 years ago and is recommended for all adolescent girls and boys 11 and 12 years old. It is approved for females between 9 and 26 and is nearly 100 percent effective in preventing pre-cancers and noninvasive cervical cancers caused by two strains of the virus.
Kentucky falls in the bottom 10 states for HPV vaccinations, with 37.5 percent of its girls and 13.3 percent of boys aged 13-17 vaccinated as of 2014.
An earlier study of adult Appalachian women aged 18-26 that were offered the first HPV vaccination free found that 45.1 percent got the first dose, 13.8 percent got the second dose and only 4.5 percent got all three doses. This and other formative research prompted the UK Center to start a two-stage HPV vaccine promotion program for women aged 19-26 in the Kentucky River Health District.
First, researchers launched a marketing campaign to recruit the women in for the first dose. Then, participants were asked to participate in the study, which was designed to promote adherence to doses two and three. The volunteer participants were randomly separated into two groups; one participated in an informational video-based intervention that was made using local people along with the traditional standard of care; the other was offered standard of care alone.
Vanderpool said the “take-home message” was that women were two and one-half times more likely to complete the series if they watched the DVD.
Since the completion of the study, 18 Kentucky health departments now use the DVD to promote completion of the three-dose HPV series, and it has also been adapted for use in North Carolina and West Virginia.
