Study finds Medicaid is paying for more emergency-room visits while charity care and self-pay visits drop
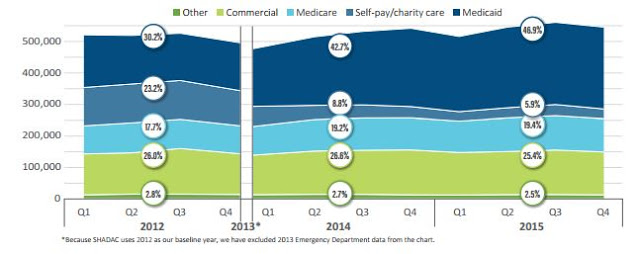
The study for the Foundation for a Healthy Kentucky found that last year Medicaid paid for 46.9 percent of ER visits, up from 30.2 percent in 2012. Conversely, charity and self-pay covered visits to the ER dropped to 5.9 percent last year from 23.2 percent in 2012.
 |
| SOURCES OF PAYMENTS TO HOSPITAL EMERGENCY DEPARTMENTS |
“We’re seeing an expected shift in payment from charity care to Medicaid in these early years of the Affordable Care Act implementation, but the ACA is only a part of the answer to reducing the volume of ER use,” Ben Chandler, president and CEO of the foundation, said in a news release.
Chandler said the state needs to enact policies to help Kentuckians establish regular doctor visits and seek preventive care. “That’s a much less expensive approach, and it results in much better long-term health than going to the hospital in an emergency,” he said.
WAVE-TV reported in August that 2.4 percent of Kentucky Medicaid’s ER costs in 2015, or $9.3 million, were for non-emergency cases.
Gov. Matt Bevin’s new Medicaid plan, which is under negotiation with the federal government, calls for up to a $75 fee for Medicaid-expansion members who use the ER for non-emergencies. Traditional Medicaid users would not be subject to the fee.
The report comes from the State Health Access Data Assistance Center at the University of Minnesota, which the foundation is paying more than $280,000 to study the impact of the federal health-reform law in Kentucky over three years. This study is a quarterly snapshot of April, May and June.
In 2014, Kentucky hospitals reported 2.1 million ER visits, which was nearly identical to the number of visits in 2012. Visits rose slightly to 2.2 million in 2015, according to the report, but it cautions, “More long-term data is necessary to determine whether that represents a year-to-year fluctuation or an actual increase.”
An earlier report from the same study found that about 29 percent of those who used the emergency department said it was because of a medical emergency. Almost 29 percent said they did so because other facilities weren’t open when they needed care, and 18 percent only named a specific health condition. Seven percent said they were following a doctor’s order, 3 percent said the emergency department was nearby, and 3 percent said they were taken by a first responder. Eight percent gave other answers.
The release notes that other studies have found a pattern of initial increase of ER use after Medicaid expansion, followed by a slowing down. It also noted that research shows that the increase in ER use cannot be primarily attributed to the uninsured.
The earlier report found that 42.4 percent of Kentuckians who used the emergency department were uninsured, 48.2 percent had public insurance and 34.1 percent had private insurance.
“ER use has been rising for two decades across the country, but it’s not the uninsured who are going more often,” Chandler said. “It’s going to take a combination of delivering care differently, ensuring that people have a regular doctor they can get in to see when needed, better care coordination, and more education before we see a sustained reduction in ER use.”