Kentucky rises to No. 3 in diabetes, increasing concern about removing dental and vision coverage from basic Medicaid
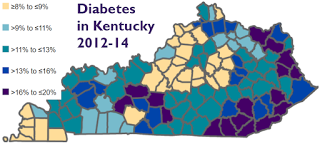
Gov. Matt Bevin’s plan for Medicaid “would have a profound effect in a state with the nation’s third-highest rate of diabetes,” The Courier-Journal reports, because it would remove dental and vision care from the regular package of benefits.
Reporter Deborah Yetter cites a Louisville optometrist who often discovers diabetes during routine eye exams, and an Eastern Kentucky dentist who “is seeing many more patients thanks to Kentucky’s 2014 expansion of Medicaid that added coverage for those he describes as the ‘working poor’.”
“Dr. Bill Collins, a dentist and president of the Kentucky Dental Association, sees many patients with diabetes, which can worsen oral health,” Yetter writes. “Some patients are in such bad shape they must have all of their teeth extracted” because, he said, they have gone “so many years without care and without insurance.”
Kentucky had the nation’s sixth highest diabetes rate until Friday, when the federal Centers for Disease Control and Prevention issued figures for 2015 and ranked the state third.
“The percentage of adults with diabetes went from 11 in 2014 to 12 in 2015, the statistics show, as the state continued to struggle with the disabling and potentially fatal disease. Only Mississippi (14) and West Virginia (13) had higher percentages,” Yetter reports. “Moreover, diabetes rates among those on Medicaid are nearly double that of the rest of the population, according to a 2015 state report” based on 2013 figures.
Dentists and optometrists asked Bevin not to remove dental and vision coverage from basic Medicaid, “arguing visits to the dentist and eye doctor are often the first step in identifying more serious health conditions, including diabetes,” Yetter notes. “But the administration made only slight changes to its proposal, allowing dental and vision benefits only for the first three months of Medicaid coverage.” Afterward, dental and vision benefits would be optional, “available only through a ‘rewards’ program where Medicaid members can earn points to pay for them through activities such as work or volunteering.”
Cabinet for Health and Family Services spokesman Doug Hogan told Yetter there would be several “easy ways” for Medicaid members to gain dental and vision coverage, including weight-loss programs and classes about diabetes.
Hogan “said Bevin’s proposal was designed to mirror commercial health plans, which do not typically include dental and vision benefits,” Yetter writes. “And Medicaid does not require dental and vision benefits to be included.”
Bevin’s proposal to the federal government “also promotes moving many people off Medicaid to commercial insurance through their employers,” Yetter notes. “Collins said the problem with the governor’s plan is that many of the adults added through the expansion work at low-wage jobs that don’t offer health insurance.”
“I don’t think they understand who they are trying to take off,” Collins told Yetter. “These are the working poor. You’re taking off working people who are trying to make a living.”
Yetter writes, “Collins said diabetes is especially problematic for people with poor oral health because it makes them more susceptible to infection, tooth decay and other oral diseases. Such patients require careful monitoring and access to regular dental care, Collins said. Without it, he worries Kentucky will never drag itself up from its low rankings in tooth decay and its high rate of toothless adults – for many a barrier to jobs or well-paying jobs.”
“I know something has to be done to address the Medicaid funding,” he told Yetter. “But we need to find ways to fund it.”
The 2014 expansion made anyone in a household with income up to 138 percent of the federal poverty level eligible for Medicaid. Before that, Yetter notes, “Medicaid was limited to very poor pregnant women and children, disabled people and low-income elderly in nursing homes.”
The federal government is paying the full cost of the expansion through Dec. 31. On Jan. 1, the state will begin paying 5 percent, rising in annual steps to the federal health-reform law’s limit of 10 percent in 2020. Bevin says the state can’t afford the cost.
