Ky. had biggest drop in uninsured low-income people, and in percentage of adults who passed up care because of cost
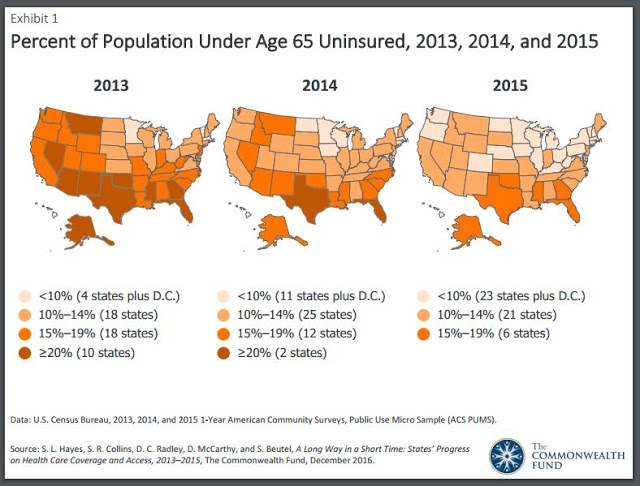
Those two findings were the Kentucky highlights of the latest Commonwealth Fund report on the impacts of the 2010 health-reform law, released Dec. 20.
The report says the uninsured rate for low-income adults in Kentucky fell 25 percentage points, from 38 percent in 2013 to 13 percent in 2015, following the state’s expansion of Medicaid under the law in 2014. Nationally, the uninsured rate for low-income adults dropped from 38 percent to 25 percent during the two-year span.
“I think this proves again what we already knew – that Kentucky has been a national model in getting folks covered,” Emily Beauregard, executive director of Kentucky Voices for Health, told Laura Ungar of The Courier-Journal.
The uninsured rate for all working-aged adults in Kentucky, regardless of income, dropped from 21 percent in 2013 to 8 percent in 2015.
The report looked at dental visits and out-of-pocket health spending relative to income to measure how states compare on access to health care. Nationally, Kentucky ranked 18th for this measure, moving up 10 spots from last year’s rankings — the largest gain in the nation.
Kentucky also improved more than any other state in the share of adults who said they went without health care because of cost. That measure dropped to 12 percent in 2015 from 19 percent in 2013. Among low-income Kentuckians, it dropped from 34 percent to 21 percent.
Kentucky is one of the states that expanded Medicaid to allow coverage to those who earn up to 138 percent of the federal poverty level. That has added about 440,000 Kentuckians to the Medicaid rolls, which now include more than a fourth of the state’s population. Under Obamacare, the federal government is paying the full cost through the end of this year. The state will have to start paying 5 percent of the cost Jan. 1, rising in annual steps to the reform law’s limit of 10 percent by 2020.
The state’s share of the cost is not financially sustainable, argues Republican Gov. Matt Bevin, who has asked federal officials to approve a Medicaid plan that largely targets “able-bodied adults” who qualify for Medicaid under the expansion. The plan includes co-pays, premiums, health savings accounts and work and volunteer requirements for those who aren’t primary caregivers. Critics of the plan say it is too complicated and creates barriers to health care.
Doug Hogan, a spokesman for the state Cabinet for Health and Family Services, told Ungar that it’s misleading to look at the uninsured rate without additional context, noting that the number of people who had private health insurance is about the same as it was before the ACA. “What we saw was an unsustainable growth of 68 percent in the state’s Medicaid program,” he said.
Beauregard argued that scaling back the Medicaid expansion and repealing the ACA, as President-elect Donald Trump and other Republicans have vowed to do, is a bad decision for Kentucky, noting that Kentucky is one of the poorest and unhealthiest states in the country.
“The gains that we’ve made are at risk,” she told Ungar, adding that charity and uncompensated care at hospitals will go up if people lose their health insurance. “There will be real consequences for the entire state of Kentucky.”
Hogan pointed out that simply having Medicaid doesn’t improve health outcomes, and said Bevin’s new plan is sustainable and “will improve the health of our citizens and encourage self-sufficiency.” He added, “We owe it to our citizens to do more than simply enroll people in social welfare.”
