Ky. was one of states helped most by coverage of pre-existing conditions; that will be a key point in Obamacare repeal debate
Kentucky Health News
Kentucky was one of the states helped most by the health reform law’s requirement that people with pre-existing conditions could get insurance – a key rule that president-elect Donald Trump says he wants to maintain while “repealing Obamacare.”
Before the law took full effect three years ago, 33 percent of non-elderly Kentuckians had pre-existing conditions that would have allowed companies to refuse to insure them, according to a report by the Kaiser Family Foundation. The only states than ranked higher were West Virginia, with 36 percent, and Mississippi, with 34 percent. Alabama also came in at 33 percent.
Kentucky’s 33 percent figure translates to 881,000 Kentuckians, just about double the number most frequently associated with the Patient Protection and Affordable Care Act in Kentucky: 440,000 Kentuckians who are on the Medicaid program because it was expanded to people in households with incomes up to 138 percent of the federal poverty level.
“To what extent people with pre-existing health conditions are protected is likely to be a central issue in the debate over repealing and replacing the ACA,” says the Kaiser report, which estimated that 52.2 million people – 27 percent of the population under age 65 – had pre-existing conditions that could have kept them from getting health insurance before 2014.
 |
| Kaiser Family Foundation chart; figures are national |
“At any given time, the vast majority of these approximately 52 million people with declinable pre-existing conditions have coverage through an employer or through public programs like Medicaid,” the report says. “In 2015, about 8 percent of the non-elderly population had individual market insurance. Over a several-year period, however, a much larger share may seek individual market coverage. This market is characterized by churn, as new enrollees join and others leave (often for other forms of coverage).
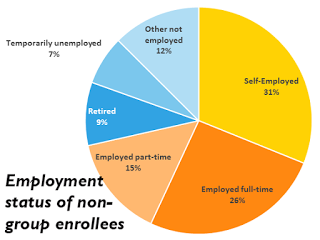
“For many people, the need for individual market coverage is intermittent; for example, following a 26th birthday, job loss, or divorce that ends eligibility for group plan coverage, until they again become eligible for group or public coverage. For others – the self-employed, early retirees, and lower-wage workers in jobs that typically don’t come with health benefits – the need for individual market coverage is ongoing.”
The figures come from the federal government’s National Health Interview Survey and Behavioral Risk Factor Surveillance System (BRFSS), polls that “can be used to estimate rates of various health conditions (NHIS at the national level and BRFSS at the state level),” Kaiser reports. “We consulted field underwriting manuals used in the individual market prior to passage of the ACA as a reference for commonly declinable conditions.”
 |
| Kaiser Family Foundation table; click on it for a larger version |
“In addition to declinable conditions, many insurers also maintained a list of declinable medications,” Kaiser notes. “Current use of any of these medications by an applicant would warrant denial of coverage.” The medications include several popular drugs used against arthritis, blood clots, diabetes, psychological and other conditions.
Also, some insurers refused to cover people in jobs deemed risky, and would charge extra, limit benefits or increase deductibles for people with conditions that could generate significant claims, including “acne, allergies, anxiety, asthma, basal cell skin cancer, depression, ear infections, fractures, high cholesterol, hypertension, incontinence, joint injuries, kidney stones, menstrual irregularities, migraine headaches, overweight, restless leg syndrome, tonsillitis, urinary tract infections, varicose veins, and vertigo,” Kaiser reports.
All this is called medical underwriting. It had many other rules, depending on insurers and state laws. The reform law’s “ban on medical underwriting also is the provision that makes Obamacare’s least popular provision — the individual mandate — essential,” writes Michael Hiltzik of the Los Angeles Times. “If insurers are required to sell coverage to all applicants at roughly the same price, then everyone must be required to buy coverage.”
Hiltzik reports that current proposals from Republicans, who control Congress, would generally “replace the individual mandate with a different incentive: It bans medical underwriting of anyone who has maintained ‘continuous coverage’ – that is, haven’t let their coverage lapse. . . . Since the primary reason people let their insurance lapse is because they can’t afford it, a default plan would have to be available at rock-bottom cost, which means a government subsidy of some sort.
Still, if congressional Republicans are as resolute as they say to repeal Obamacare, the medical underwriting ban may have to go, or at least be seriously eroded.”