Ky. and most surrounding states had fewer companies on government health-insurance exchanges this year than last year
 The number of health insurance companies offering subsidized coverage didn’t shrink just in Kentucky, but in most of adjoining states, according to a study done for the Foundation for a Healthy Kentucky.
The number of health insurance companies offering subsidized coverage didn’t shrink just in Kentucky, but in most of adjoining states, according to a study done for the Foundation for a Healthy Kentucky.
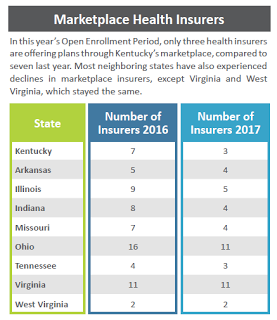
The report found that the number of insurers on Kentucky’s exchange dropped to three in 2017 from seven in 2016. Likewise, the number of insurers in Illinois and Indiana also dropped by four. Ohio’s exchange lost five insurers during this time frame, but it still has 11 to choose from. Virginia, with 11, and West Virginia, with 2, remained the same.
The report found that while Kentucky continues to have three insurers on the exchange, only one of them covers all 120 counties, leaving 59 counties with one carrier, 52 counties with two carriers and only nine counties with all three.
“One of the concerns about the uncertainty surrounding the Affordable Care Act is that the number of insurers offering plans is dwindling in many markets, and that’s exactly what happened in Kentucky,” Ben Chandler, president and CEO of the foundation, said in the news release. “Kentuckians living in more than 90 percent of counties in the commonwealth had just one or two carrier choices; half of Kentucky counties had only one carrier option. And the choices were most limited in the lower-income, less-healthy areas of the commonwealth.”
The ACA requires everyone to be covered by health insurance, either public or private, or pay a penalty. Consumers who buy plans on the exchange, depending on their income, may be eligible for tax credits to reduce their monthly premium payment amounts.
The report also found that in 2017, the second-lowest priced silver-level plan for a family of four with an income of $60,000 was lower in Kentucky than both the U.S average and five of its eight neighboring states, though the monthly premium cost for all of the states in the study was about the same, around $405, after the varying amount of tax credits was subtracted from the varying premium costs.
 For example, Kentucky’s premium for this plan is $939, and the tax credit is $534, leaving the person to pay $405 each month. The U.S. average premium for this plan is $1,090, with a tax credit of $686, leaving the person to pay $404 each month.
For example, Kentucky’s premium for this plan is $939, and the tax credit is $534, leaving the person to pay $405 each month. The U.S. average premium for this plan is $1,090, with a tax credit of $686, leaving the person to pay $404 each month.
Chandler said that fewer carriers lead to higher premiums, less competition, and higher cost to taxpayers who pay for the tax credits to buy those premiums down.
He also pondered what would happen if insurers refused to cover some areas of the state altogether, thus removing any opportunity for a tax credit for those residents and making it more expensive for them.
“That would move Kentucky backward by once again increasing the number of people who cannot afford insurance, so they rely on the emergency room or just delay or skip essential health care,” he said.
The study was done by the State Health Assistance and Data Center at the University of Minnesota.
