Though more have insurance and can see a doctor, Ky. shows little gain on health outcomes; Chandler says that takes time
Kentucky Health News
The percentage of Kentuckians without health insurance has dropped by more than half since the implementation of the Patient Protection and Affordable Care Act three years ago, and few of the insured are having trouble finding a doctor when they need one, according to a report for the Foundation for a Healthy Kentucky.
However, the report also said little progress has been made to improve Kentuckians’ health-care quality and health outcomes since the law was fully implemented in 2014.
“The ACA has led to clear progress for many Kentuckians in three of the five areas we tracked: insurance coverage, access to regular doctor visits and health-care costs for families,” said Ben Chandler, president and CEO of the foundation. As for health-care quality and outcomes, he said, “Often, it takes longer to see these results; you don’t turn around low birth weights or lengthen average lifespans in a couple of years.”
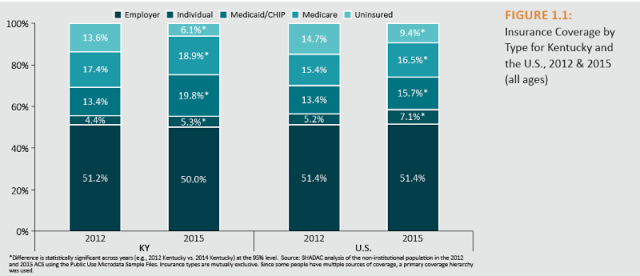
The report found that since the implementation of the ACA, Kentucky’s uninsured rate dropped to 6.1 percent from 13.6 percent. The highest coverage increase came in Medicaid and the Children’s Health Insurance Program; 13.4 percent of Kentuckians had such coverage in 2012, and 19.8 percent had it in 2015.
Kentucky and other states that fully expanded Medicaid under the ACA saw the greatest increases in coverage. Neighboring states that expanded Medicaid had uninsured rates of 7 percent or lower; those that didn’t, such as Tennessee, had rates of 9.1 percent or higher. It also noted that two neighboring states that expanded Medicaid through an “alternative” approach, like Kentucky has proposed to do, have uninsured rates similar to the non-exemption states.
The report also found that more Kentuckians said they had seen a health-care provider in the year prior to being surveyed (73.8 percent in 2012, rising to 78.7 percent in 2015) and fewer Kentuckians said they were delaying or skipping health care because they couldn’t afford it (dropping from 11.7 percent to 6.5 percent). However, this wasn’t true for the poorest and sickest Kentuckians who said health care cost still kept them from getting the care they needed.
Contrary to assertions by Republican Gov. Matt Bevin, the report says there is no evidence that the newly insured in Kentucky are having trouble finding a doctor when they need one, nor have they had an increase in average out-of-pocket spending on health care since 2012.
“Nearly 95 percent of Kentuckians could still find a doctor when they needed one,” said Chandler, who voted against the ACA when he was a Democrat representing the 6th District in 2009.
Other improvements included fewer elderly Kentuckians delaying prescription refills or skipping or reducing medication doses because of high drug costs; a more than 500 percent increase in the number of covered substance-abuse treatments through Medicaid; a drop in the number of Kentuckians having trouble paying their medical bills; and lower monthly premiums in Kentucky’s marketplace compared to most surrounding states and the U.S.
The report also looked at “quality-of-care” indicators and found they had neither improved nor declined since the ACA was implemented.
It noted that three of the quality measures that they looked at had “shown some progress,” including the number of infants who were breastfed at discharge from the hospital, preventable hospitalizations due to high blood pressure, and asthma and colorectal screenings. It also noted that the state’s smoking rate had dropped from 28.3 percent in 2012 to 26 percent in 2015, though the high-school student smoking rate had a smaller decline, from 17.9 percent in 2013 to 16.9 percent in 2015.
The report cites negative trends related to health behavior. Preventable hospitalizations due to short-term complications from diabetes increased, and the state’s obesity rate rose from 31.3 percent in 2012 to 34.6 percent in 2015.
Chandler noted that some health measures, especially related to chronic health issues, may have worsened at first but then improved because many Kentuckians were seeing providers for the first time and were newly diagnosed. He noted that this increased access to care will ultimately improve the health of Kentuckians and decrease health care cost in the future.
“Myriad factors contribute to health and it takes time to change the tide in health outcomes,” Chandler said. “In the long run, though, increased coverage, improved access and lower costs lead to better quality and outcomes. That’s why I’m grateful Kentucky continues to support Medicaid expansion. We all want to sustain the gains we’ve achieved under the ACA and see the long-term benefits of increased coverage and access.”
The foundation’s study on the impact of the ACA over its first three years in Kentucky was conducted by the State Health Access Data Assistance Center at the University of Minnesota. Click here to see the full report.
