UK and Norton hospitals rank high in resistant bloodstream infections; UK cites complex cases, recent improvements
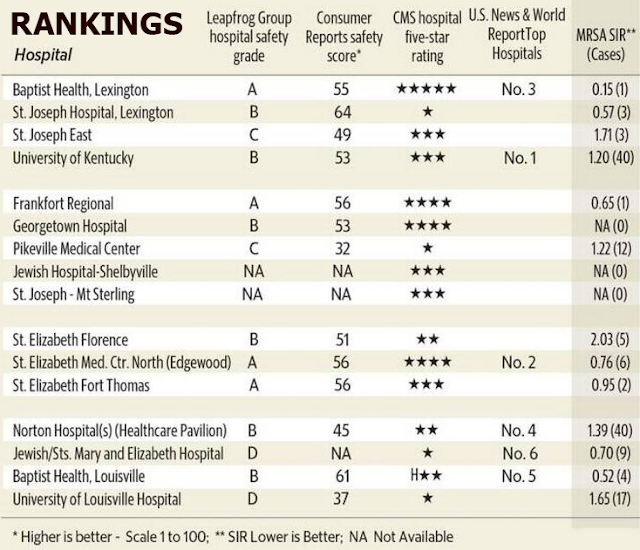
“Kentucky’s two biggest hospital systems had some of the country’s highest instances of an often deadly bacterial bloodstream infection known as MRSA” in the fiscal year that ended June 30, 2017, Linda Blackford reports for the Lexington Herald-Leader.
The Albert B. Chandler Hospital at the University of Kentucky and Louisville’s Norton Healthcare each had 40 bloodstream infections of methicillin-resistant staphylococcus aureus, according to the Centers for Medicare and Medicaid Services. Of the 3,800 hospitals reporting, Norton and UK ranked sixth and seventh, respectively.
Officials from both hospitals told Blackford that they follow precautions recommended by the federal Centers for Disease Control and Prevention, and that using the raw number of cases can be misleading because it doesn’t take into account how many patients are admitted each year and how long they stay.”At UK HealthCare, we take quality and safety very seriously and have implemented multiple processes to help reduce the number of infections to keep patients safe,” spokeswoman Kristi Willett told Blackford. “Our large patient volumes and high level of patient complexity make us unique in the state of Kentucky as those things are known risk factors that can increase the risk of infection.” MRSA is resistant to most antibiotics, and is most dangerous as a bloodstream infection.
UK handles many of the state’s most complex medical cases, which require longer stays, making them more vulnerable to infection, said Derek Forster, UK’s medical director for infection prevention and control. He said that since 2016, when it added precautions for patients in intensive care, the hospital’s “standardized infection ratio” is down 55 percent, and MRSA infections in its ICUs have been reduced by half.
Norton’s chief medical officer, Steven T. Hester, “said Norton noticed an increase in MRSA cases in 2016, and convened a system-level task force to deal with the issue,” Blackford reports, quoting him: “Unfortunately, Kentucky is a state with a high incidence of opioid and intravenous drug abuse. We had concerns that our increase in MRSA could be related to the increased incidence and risk with substance dependent patients, specifically intravenous drug users.”
Blackford reports, “Among other hospitals in Kentucky, the University of Louisville Hospital had 17 MRSA cases, Pikeville Medical Center had 12 and Hazard ARH had 10 cases. Hazard’s number was deemed to be ‘worse than the national benchmark.’ Most of Kentucky’s small, regional hospitals had fewer than five cases.”
“Hospitals can and must do better,” retired Somerset physician Kevin Kavanagh, board chair of Health Watch USA, writes in an op-ed for the Herald-Leader, in which he takes a close look at hospital ratings, especially on safety issues.