Federal judge blocks new Medicaid plan, which was to go into effect Sunday
By Al Cross
Kentucky Health News
A federal judge has blocked Kentucky’s new Medicaid plan, which was to go into effect Sunday, July 1.
U.S. District Judge James Boasberg of Washington, D.C., vacated the U.S. Department of Health and Human Services‘ approval of the plan, saying federal officials “never adequately considered whether” it “would in fact help the state furnish medical assistance to its citizens, a central objective of Medicaid.” Calling that a “signal omission,” Boasberg declared the waiver of normal Medicaid rules “arbitrary and capricious,” keys for overturning an administrative decision.
The plan calls for Medicaid members to pay small, income-based premiums, and has “community engagement” requirements for “able-bodied” members who are not primary caregivers: work, volunteering, job training or drug treatment at least 80 hours a month.
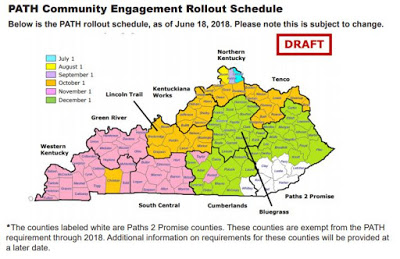
The community-engagement rules were to be phased in, starting in Campbell County on Sunday and in all but eight counties by Dec. 1.
Lawyers for the 16 Kentucky Medicaid members who filed the suit argued that the plan was not likely to promote the objectives of the program, and that Health and Human Services Secretary Alex Azar “entirely failed to consider” or alter the state’s projection that in five years, Kentucky Medicaid would have 95,000 fewer members than it would without the waiver. Academic health experts said in a friend-of-the-court brief that a more likely range was 175,000 to 297,500.
Medicaid covers 1.4 million Kentuckians, almost half a million of them under the previous state administration’s 2014 expansion of eligibility to people with incomes up to 138 percent of the federal poverty level, as provided by the 2010 Patient Protection and Affordable Care Act. Most on the expansion work.
“The record shows that 95,000 people would lose Medicaid coverage, and yet the secretary paid no attention to that deprivation,” wrote Boasberg, who was appointed by Barack Obama. Actually, the state’s projection is not that 95,000 particular individuals will lose coverage, just that the rolls would be that much lower than otherwise. That many people enroll in or go off Medicaid in just a few months; the program has a lot of what officials call “churn.”
The state said in its application that some of the reduction would be a result of members not complying with requirements of the program, which include regular reporting and premium payments. Violation would result in a six-month “lock-out” from the program, unless the member completed a course in health literacy or financial literacy. The Kaiser Family Foundation has estimated that a clear majority of lock-outs would be a result of failure to report.
Boasberg noted that experts who submitted comments to the state and HHS cited “extensive research, including from past Medicaid demonstrations . . . would likely reduce health-care access and utilization. To top it off, numerous comments also suggested that these new administrative requirements would increase “clerical and tracking errors and delays,’ which in turn would ’cause inadvertent terminations’.”
The requirements for work or other “community engagement” activities were to take effect in Campbell County Sunday, July 1. They are part of a plan the state calls Kentucky HEALTH, for “Helping to Engage and Achieve Long Term Health.”
Boasberg’s ruling sends the issue back to HHS for review. State Health Secretary Adam Meier issued a statement calling Boasberg’s ruling “very narrow” and saying the state would work with the Centers for Medicare and Medicaid Services “to quickly resolve the single issue raised by the court so that we can move forward with Kentucky HEALTH.”
However, other issues may stand in the way. Boasberg said he didn’t have to rule on some issues raised by the plaintiffs because Azar’s omission was enough to invalidate the waiver.
Meier added, “Without prompt implementation of Kentucky HEALTH, we will have no choice but to make significant benefit reductions.” He told a legislative committee June 20 that in case of an adverse ruling, the state would likely have to cut dental, vision and possibly prescription-drug coverage for some people. Kentucky HEALTH had already shifted dental and vision benefits from being free to an option that requires members to participate in certain activities.
The state is expected to appeal Boasberg’s ruing; Gov. Matt Bevin has said the issue will ultimately be decided by the Supreme Court. Bevin said in his executive order for the plan that if courts ruled against it and the state’s appeals failed, six months later the Medicaid expansion would end.
“Bevin is trying to take Medicaid expansion hostage, arguing that if Kentucky isn’t allowed to impose a work requirement, then there will be no more expansion,” writes Dylan Scott of Vox. “By the Bevin administration’s logic, work requirements do advance the goals of Medicaid, because without them, Kentucky is going to end its expansion and hundreds of thousands of the state’s most vulnerable citizens will lose their insurance.”
Kentucky is one of four states where HHS has approved Medicaid work requirements. “Seven others — Arizona, Kansas, Maine, Mississippi, Ohio, Utah, and Wisconsin — have proposals waiting for approval,” Scott reports.
Boasberg’s decision is at https://ecf.dcd.uscourts.gov/cgi-bin/show_public_doc?2018cv0152-74.