Ky. making great strides in treating patients with hepatitis C, with harm-reduction programs and fewer restrictions on treatment
By Melissa Patrick
Kentucky Health News
Eliminating hepatitis C in Kentucky and the rest of the nation will require universal screening and non-restricted access to treatment, and because new cases of the disease are largely driven by intravenous drug use, states must also commit to increasing harm-reduction programs like syringe exchanges and medication assisted therapies.
Those were the overarching messages to more than 300 people who attended the fifth annual Viral Hepatitis Conference in Lexington on July 31. The good news was that Kentucky has made great strides on all of these fronts since last year’s conference, which had a similar message.
Access to harm reduction is one of the areas in which Kentucky has excelled.
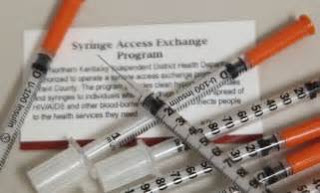
Dr. Allen Brenzel, medical director for the Department of Behavioral Health and Developmental Disabilities, told the crowd that one of the things he was most proud of was the state’s syringe exchanges, which are mainly intended to decrease the spread of infectious diseases, such as hepatitis C and HIV.
Kentucky leads the nation in the number of counties with local syringe exchanges. As of July, 45 of the state’s 120 counties have approved such programs at more than 50 sites. That’s a lot more than Brenzel expected under a 2015 law that requires approval by the local health board, the county fiscal court and governing body of the city where the exchange is to be located.
“I travel a lot, and the fact that Kentucky has harm-reduction syringe exchange is one of the things I’m most proud of . . . It’s an incredible thing,” Brenzel said. “We all thought we’d have four or five of them in our urban areas, but what I think is exciting is that our rural counties stood up and said, ‘We’re tired of this. We’re tired of our neighbors dying; we’re tired of our friends [dying]. We know this is a health risk.'”
Only about 10 percent of syringe-exchange participants agree to be tested for hepatitis, and critics of the programs claim they enable drug use. On the recent KET program “Disrupting the Opioid Epidemic,” host Renee Shaw asked Jennifer Hancock, president and CEO of Volunteers of America Mid-States, about that.
“It is enabling people to take that first courageous step toward a path of recovery,” Hancock replied. Earlier, she said, “They are absolutely saving people’s lives.”
Hancock, Brenzel and Dr. Ardis Dee Hoven, an infectious disease specialist with the state Department of Public Health, said the exchange specialists strive to build long-term relationships with their clients, making it easier to eventually steer them toward treatment.
“This is not about a supply of needles,” Brenzel said. “This is about the first step in the road to recovery.”
At the conference, Brenzel also talked about the state’s many different programs that are set up to distribute naloxone, the life-saving drug that can reverse the effects of an opioid overdose. Brenzel added that the U.S. surgeon general has said that having access to naloxone and learning how to use it is “as important as learning CPR.”
Jon Zibbell, senior public health scientist at RTI International, an independent nonprofit research institute, told conference attendees that the nation has both a health-care crisis and a public-health crisis.
He said that while it’s important to treat the 4 million people who are chronically infected, especially because we know that between 8,000 and 10,000 of them will die annually from a liver-related illness, it is the IV drug users with hepatitis C who are creating the public health crisis.
“The only real way to address the public health crisis for hepatitis C and hepatitis B is to address the people who are still injecting, to protect those downstream transmissions,” Zibbell said.
On top of treating people who are actively using drugs, he said, the best way to treat these individuals may be to create a “one-stop-shop” for related services, including hepatitis C treatment, medication-assisted therapies, syringe exchange and access to naloxone.
“We need a way to make it so infected people don’t transmit the virus and uninfected people don’t acquire the virus, and then naloxone to keep them alive,” he said.
Kentucky no longer requires people getting hepatitis C treatment to stay off illicit drugs, only that they be screened and counseled for any illicit drug use. The state has also removed the requirement that only allowed treatment during advanced stages of the disease; now anyone can be treated for it.
The state still requires the disease be treated by or in consultation with a specialist, which is a challenge because there aren’t enough specialists to meet Kentuckians’ needs.
Dr. Jens Rosenau, an associate professor of medicine at the University of Kentucky and a hepatologist and gastroenterologist at the Kentucky Clinic, said that between July 2014 and December 2016, before the restrictions were removed, only 22 percent of his patients started treatment for the disease, largely because of the restrictions.
But after the majority of the state’s managed-care organizations lifted the restrictions in April, allowing Medicaid to pay for treatment, he said his treatment uptake rates have doubled. “This month we actually started 150 patients on treatment,” he said. “It is probably our record now.”
Rosenau also noted that the UK Healthcare emergency department started doing universal screening for hepatitis C in July and that in just two weeks had identified more than 70 patients with the disease who didn’t know they had it: “That is overwhelming.” The disease is common, but latent, among the Baby Boom generation.
Kentucky is also the first state in the nation to pass a law that requires all pregnant women to be tested for hepatitis C, and for their babies to be tested at 24 months if the mother tested positive. One in 56 Kentucky births are to mothers who have hepatitis C.
Barbara Cave and Danielle Revert, family nurse practitioners in Louisville, said the state needs universal screening for hepatitis C.
Revert noted a study found that using the current guidelines for screening, 25 percent of people who would test positive for the disease would be missed. “If we’re going to talk about eradicating this disease, I really think we’re going to have to shift our screening focus more toward this universal screening idea,” she said.
Cave added that the prevalence of hepatitis C is likely far greater than the 3.5 million that is normally reported because this number doesn’t include any people who are institutionalized, incarcerated, hospitalized, homeless or are military veterans. She said the U.S. estimate should be closer to 5.2 million.
Corinna Dan, viral hepatitis policy adviser for the U.S. Department of Health and Human Services, said it’s challenging to get people to pay attention to a specific health issue like hepatitis, and that it simply doesn’t have the kind of support that you see for many other health conditions, like HIV, which has a “huge advocacy base.”
“We haven’t done that yet effectively for hepatitis,” she said. “We do need champions at the ground level, at the local level . . . because that’s where people are served, that’s where people have the need.”