Report offers five strategies to fight opioid epidemic in Appalachia; central part of region had high death rate from overdoses

By Melissa Patrick
Kentucky Health News
The third report in a series that offers “replicable best practices” for Appalachian communities to improve their health offers strategies to address the opioid epidemic, which has swept through much of the region. The other two address smoking and obesity.
The report, Health Disparities Related to Opioid Misuse in Appalachia, Practical Strategies and Recommendations for Communities was created by the Appalachian Regional Commission and the Foundation for a Healthy Kentucky, and also funded by the Robert Wood Johnson Foundation.
Prior research sponsored by ARC shows that residents of Appalachia are more likely to die prematurely than those who live outside the region. And while the report recognizes that multiple factors contribute to this, it says, “Notable trends in opioid-related deaths significantly contribute to the loss of life in Appalachia.”
The report says the poisoning-mortality rates in Appalachia is 20.4 per 100,000 residents, compared to 14.4 elsewhere. The rate is 36.6 in Central Appalachia, the ARC subregion that includes all of Kentucky’s Appalachian counties. The report points to four Appalachian states, West Virginia, Ohio, Pennsylvania, and Kentucky, which have some of the highest rates of drug overdose in the country.
The report focuses on five specific recommendations in the areas of prevention, increased access to treatment and recovery for opioid-use disorders, harm reduction, long-term recovery supports, and community-based solutions.
“While our nation’s opioid crisis seems to have most significantly impacted Appalachia, I believe the region can be known as a leader in innovative solutions to this pervasive threat to communities throughout our country,” ARC Federal Co-Chair Tim Thomas said in a news release. “I am pleased to see such efforts ongoing in the region, and I hope that the information provided in this brief will help other communities as they work to strengthen their response to this epidemic.”
Before implementing any of the recommended strategies, the report first encourages communities to do a “community needs assessment” to better understand the cultural norms and attitudes around opioid-use disorder and opioid overdoses. The report offers tips on how to do such an assessment, state- and county-level health data, and funding strategies to pay for opioid-related initiatives.
Youth prevention strategies are discussed in detail in the report, including one in McCreary County that is led by the Adanta Regional Prevention Center that has helped its schools implement a teacher-led evidence-based drug prevention program.
The report also encourages increased use of the the prescription drug monitoring programs as a way to decrease the over-prescribing of opioids in the region. The report says a “gold standard” for monitoring if Kentucky’s KASPER system, which stands for Kentucky All Schedule Prescription Electronic Reporting.
Another recommendation in the report is to make sure providers understand the appropriate use and dosing of prescription opioids, which continues to be a problem. Kentucky passed a law in 2017 to address this issue that limits most painkiller prescriptions to a three-day supply for acute pain, but it passed with a long list of exceptions and some have suggested that it is not being strictly adhered to.
Strategies to increase access to treatment for opioid use disorder include increasing access to medication-assisted treatment. MAT combined with counseling is considered the gold standard of treatment for opioid-use disorder. Three MAT drugs have been approved, including methadone, buprenorphine and naltrexone.
“To improve access to MAT, communities may seek to increase the number of providers who offer MAT, invest in telehealth programs and integrate behavioral health into primary care and emergency department settings,” says the report.
The report also notes the importance of harm-reduction programs. These include syringe exchange programs, the distribution of naloxone, safe drug disposal programs and the prevention and treatment of neonatal abstinence syndrome.
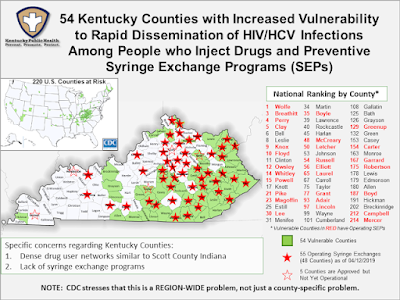
In Kentucky, local governments have approved 52 syringe exchanges, with all but four of them operational. However, about 54 counties that are considered at high risk for HIV and hepatitis C outbreaks among IV drug users still don’t have one — and most of those counties are in Appalachia.
The report encourages the use of drug courts, which are designed to get people with opioid-use disorders into treatment and out of the criminal justice system. Kentucky recently implemented an educational program, called RESTORE, to teach judges and the court staff about opioid-use disorders, treatment and recovery as a way to help them make informed decisions in related cases.
It also points out that supporting long-term recovery for people with opioid-use disorders often involves helping them with “upstream factors,” like housing or jobs or passing policies that support them. It also notes the value of providing access to peer support specialist, who can act as mentors to people with opioid-use disorders.
Additionally, it stresses the importance of forming community coalitions that brings everyone to the table to address this issue, including law enforcement, social service providers, schools, health providers and policymakers.