National foundation study estimates Medicaid work rules would lead to 86,000 to 136,000 in Ky. losing coverage the first year
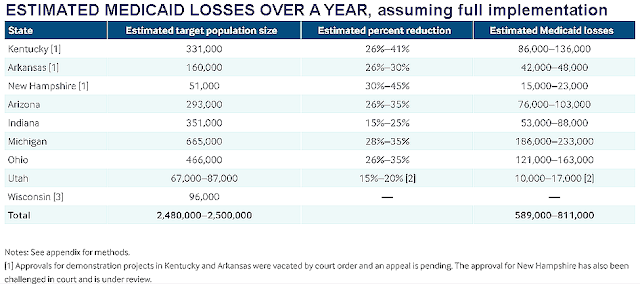
Commonwealth Fund chart, adapted by Kentucky Health News; click on it for a larger version
—–
If Kentucky and eight other states persuade federal courts to let them add work requirements to their Medicaid programs, Kentucky would lose more people from its Medicaid rolls than any of the states but Michigan, says a study by The Commonwealth Fund, a New York City-based foundation.
“These are losses only associated with the work requirements, and do not account for other elements like monthly premiums or new paperwork requirements that may trigger additional losses,” researchers Leighton Ku and Erin Brantley write for the fund, which says it exists to “promote a high performing health care system that achieves better access, improved quality, and greater efficiency, particularly for society’s most vulnerable and the elderly.”
Ku is director of the Center for Health Policy Research, and Brantley is senior research associate, in the School of Public Health at George Washington University in Washington, D.C.
They write, “Most adult Medicaid beneficiaries work or are limited in their ability to work because of health problems, schooling, child care, or other needs. Many who would lose Medicaid eligibility are working or trying to work, but are unable to comply with the rules because they face major barriers to steady employmentor cannot navigate the procedural barriers.”
In Arkansas, the only state that has terminated people for not complying with work rules, 18,000 lost coverage in the first six months before a federal judge blocked the program. He has also kept Kentucky from starting its program. The rulings have been appealed.
Kentucky officials say they don’t expect the state to see the results Arkansas did, largely because they have an aggressive outreach campaign and are committed to changing tactics if they see too many dropping off the Medicaid rolls. They say Kentucky’s rollout has been longer than that in Arkansas, giving more preparation time; and they have strategic partners committed to the program’s success, such as the Foundation for a Healthy Kentucky, employers and regional workforce boards.
Seven other states have federal authorization for work requirements: Arizona, Indiana, Michigan, New Hampshire, Ohio, Utah and Wisconsin. They “are either just starting to phase in their programs or have not yet begun to do so,” James Romoser reports for Inside Health Policy. The study “is based on the initial coverage losses that occurred in Arkansas . . . as well as the national effects when similar work requirements were added to the Supplemental Nutrition Assistance Program” and policy differences among the states. “The smallest impact is expected in Wisconsin, because its waiver permits 48 months of non-compliance before beneficiaries are penalized. As a result, the researchers said significant coverage losses due to work requirements might not occur in the first year.”
The director of Kentucky’s program, Kristi Putnam, says Medicaid and SNAP offer different benefits and should not be compared. She told Kentucky Health News that because American health benefits are typically tied to hours worked, it is important to help Kentuckians learn that system.