In southeastern Kentucky’s Covid-19 hotspot, health-care providers try to fight misinformation without confrontation

Martin and Joyce Huff (Photo provided)
—–
By Jamie Lucke
Kentucky Health News
Martin Huff of WYGE Christian Radio in London says he never shied from vaccines before. He gets an annual flu shot and has been vaccinated against shingles.
Covid-19 was different.
“There was so much propaganda and talk, you didn’t know what to do. People don’t know what to do.”
Huff was concerned that the vaccines had only emergency authorization from the Food and Drug Administration. “I just waited. I just waited too late, to be honest with you.”
In early July, he was diagnosed with Covid-19 and received monoclonal antibodies which, like the vaccines at the time, have emergency FDA authorization. (The antibodies must be administered soon after symptoms begin, so don’t wait to get tested.)
The virus more severely infected his wife, Joyce Huff, a nurse and supervisor at a hospital in Cincinnati.
“My wife was a no-vaxxer. She said, ‘I’m not a no-vaxxer anymore.’ It makes a believer out of you,” Huff said by telephone on Aug. 16. He said he plans to get the vaccine, but must wait 90 days after receiving the antibodies.
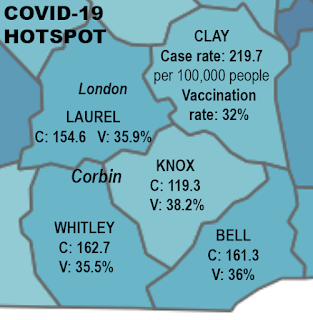 |
| Ky. Health News chart; color reflects county vaccination rate |
Baptist Health Corbin, where Huff was treated, serves counties with low vaccination rates and high infection rates.
Just one of every three residents of those counties had at least one dose of the vaccine, compared with more than half of all Kentuckians. (Children under 12 are not yet eligible to be vaccinated.)
Fueled by the more contagious Delta strain, this surge is striking younger unvaccinated adults and children, amid growing evidence that Delta is also making people sicker.
Clay County is suffering Kentucky’s highest infection rate, and one of the nation’s highest: 194.5 per 100,000 residents, more than two and a half times the state rate of 76.9.
Corbin is the seat of Whitley County, which had 167.4 cases per 100,000, third highest in the state.
London is the seat of Laurel County, where there were 153.9 cases per 100,000, seventh highest.
Kentucky Health News talked to four people on the front lines in this hotspot about their race against the deadly virus and the endless stream of misinformation that gives it an edge.
What do they say to people, who like Huff, are understandably confused and hesitant?
Spoiler alert: Their unanimous advice is to get the vaccine. Or, as Huff says, “If you know you can keep yourself from dying, you should.”
The doctor
“It frustrates me that this disease has become political, because disease has no politics,” says Dr. Shelley Bundy Stanko, chief medical officer at CHI Saint Joseph London and medical director of the Laurel County Health Department.
She tries to reassure patients that the vaccine is safe and necessary by being “very fact based” and conveying “very strongly that I think it’s best for them. I’ve had lots of long conversations about it over the last six to eight months.”
 |
| Shelley Bundy Stanko, M.D. |
Some of the unvaccinated are waiting to gather more information, and do eventually decide to get the shots. Others – probably the majority – are “sort of shutting down and not absorbing the information. It’s heartbreaking. Whether because of personal biases or politics, they have stopped listening to the medical facts.”
She’s not giving up. “Confrontation does not help. Keep the door open. Let me talk this through with you.”
She assures her patients and coworkers that the 4.8 billion doses administered worldwide provide ample proof. “We know they’re safe; we know they help.”
To patients who point out that even vaccinated people can get and spread the virus, she explains that vaccinated people become infected much less often, don’t get as sick, and recover faster.
On Aug. 17, the 150-bed London hospital was caring for the most Covid patients ever and had its highest percentage yet in intensive care and on ventilators. Even in intermediate care, Covid patients require more hands-on attention; the virus leaves them too fatigued to even feed themselves or walk to the bathroom at a time when London has not been spared from the nationwide shortage of nurses.
The rise in Covid hospitalizations is jeopardizing other patients. Stanko said it has become “extremely difficult” to find a hospital for patients who need to be transferred for specialty care, despite an effective coordination system among Kentucky hospitals.
Stanko, her husband and their three children are all vaccinated and wearing masks in indoor public places. Masking in schools is an important tool, just like booster seats and seatbelts, for keeping children safe, she said: “Even imperfectly applied,” masks on kids produce benefits and are “worth it.”
She urges people to research the facts rather than relying on “a neighbor, social media account or television channel.”
“I’m a person of faith. . . . Those of us who can be vaccinated should do it for our neighbors.”
The nurse and the chaplain
Jasmine Whitaker, a registered nurse at Baptist Health Corbin, has had nightmares about struggling into her protective gear while a monitor keeps dinging a warning that one of her patients is nosediving.
Caring for Covid patients, “you have this anxiety constantly. It doesn’t just go away when you get to the parking lot.”
Eighteen months into the pandemic, she’s coming to terms with a new wave of disease and death, one that could have been avoided, if only enough people had gotten the vaccine.
“I think sometimes you do feel, not angry, but upset, because it’s so simple to help stop the spread of Covid,” she said. “We’re aware that vaccines have side effects, but so do your daily medications. Health-care workers just had a lot of hope that more people would get the vaccine. So you kind of feel let down.”
 |
| Baptist Health Corbin has 273 beds. |
Her colleague, the Rev. Alice Tremaine, advance-care planning coordinator and a chaplain at the Corbin hospital, shares her disappointment at being “back at square one.”
“I think a lot of people think only in terms of their risk for dying of Covid. I’m hearing reports about younger people, healthier people getting permanent lung damage. A lot of people are living with really serious long-term side effects from having had Covid, needing a lung transplant when they’re young, a drastic life change in their 30s.”
Both women see families struggle with decisions when loved ones will never be able to breathe naturally again and are unaware and unable to decide for themselves. “Especially if they’re younger,” Whitaker says, “they haven’t had those kinds of conversations with family about what they would want.”
Tremaine says she sees Covid compounding the guilt and shame that people often feel in response to any premature or preventable sickness or death. “It’s become such a divisive topic. You cannot prevent the spread of Covid 100 percent. Some precautions you can take are very simple and easy, like getting vaccinated, wearing masks or social distancing. When people have failed to do that, I think there’s an extra layer of regret or even anger with each other when family members disagree about what should have been done.”
The hospital administrator
“People have asked, ‘what can we do?’ We appreciate the food and cards. But what health-care workers need more than anything is for people to get vaccinated,” says Anthony Powers, president of Baptist Health Corbin.
The largest hospital between Lexington and Knoxville is vaccinating more people – almost 100 a day vs. “in the teens five or six weeks ago,” Powers says, but the uptick is not enough to defeat the Delta strain.
Nurses are working extra shifts. The emergency room is treating record numbers, not just for Covid but people who are sick because they deferred care during the pandemic. Patients who need to be transferred for specialized or higher-level care must wait longer in the ER because other hospitals are full.
What Powers is not seeing is admissions of vaccinated people. Only two of the hundreds who have been hospitalized in Corbin for Covid have been vaccinated.
A clinic staffed by three retired nurses is infusing about 20 outpatients a day with monoclonal antibodies, the experimental treatment that then-President Trump received.
“We’ve not had anybody say no to monoclonal antibodies because it’s experimental.” Yet, there is great resistance to vaccination, which is not.
“Some pushback” has greeted the mandate that all hospital employees be fully vaccinated by the end of October or be tested at least once a week, Powers said.
“If one of our health-care workers brought it in, there could be grave consequences for patients and their families,” Powers said. “We’re a place of healing. We also want to be role models.”
Bottom line, he says: “We’ve got to get more people vaccinated.”