Ky. health-system performance ranked 41st, Covid-19 response 49th; highest hospitalization rate, relatively low vaccination rate
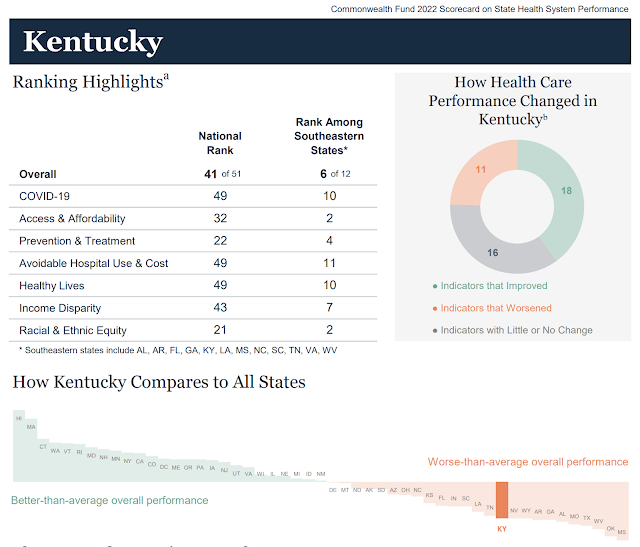
Chart from 2022 Scorecard on State Health System Performance, The Commonwealth Fund
—–
By Melissa Patrick
Kentucky Health News
Kentucky ranks 41st among the states and Washington, D.C. in the latest ranking of states’ health systems, but when it comes to how well those systems and their states’ populations have handled the pandemic, Kentucky ranked 49th, ahead of only Alabama and Oklahoma.
The rankings are done annually by The Commonwealth Fund, a New York-based foundation that says it aims to promote a high-performing health-care system. In past years, the Scorecard on State Health System Performance has asked three questions:
- Do Americans have good access to health care? Does their health insurance enable them to get the care they need to stay healthy? Are they protected from high out-of-pocket health costs?
- Are Americans getting the right health care, at the right time, and in the right setting? To what extent are they seeking care from emergency departments or other costly settings instead of visiting a primary care provider? Has health care use and spending gone up or down?
- How healthy is America? How prevalent are high-risk behaviors like smoking or health conditions like obesity that put people at higher risk for poor health? What are Americans’ chances of dying early in life from preventable or treatable causes?
This year, the fund added a question: “How well has each state responded to and managed the Covid-19 pandemic?”
“Covid-19 has disrupted aspects of care and we wanted to take a closer look at how states have responded,” said David Radley, senior scientist at the fund, said in an online press briefing.
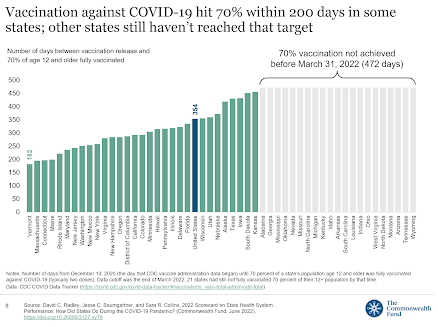
To do that, the researchers used seven metrics for Covid-19 through March 2022: hospitalization rates (Kentucky was No.1), stress on intensive-care units, hospital staffing shortages, deaths in nursing homes and overall, percentage of adults vaccinated and boosted, and the number of days it took to get 70% of the state’s 12-and-over population fully vaccinated. Kentucky is one of 21 states that still hasn’t achieved that.
While the scorecard is for state health systems, Radley acknowledged that it also reflects the choices of a state’s residents. Noting Kentucky’s relatively low vaccination rate, he said that even if the state made a strong effort to get Kentuckians vaccinated, “People also have to be willing to get the shot.”
Kentucky’s top rankings were in racial and ethnic equity (21st), prevention and treatment (22nd), and access and affordability (32nd). It ranked 43rd for income disparity, and ranked 49th in three measures: Covid-19, avoidable hospital use and cost and healthy lives. The last four are reflections of the state’s low health status, which the report ranked second from the bottom.
Among indicators used to measure the above categories, Kentucky’s best were its percentage of home- health patients with improved mobility, ranked 10th; the infant death rate (11th) and percentage of uninsured adults (12th). The state’s expansion of Medicaid under the Patient Protection and Affordable Care Act gave it perhaps the nation’s largest reduction in the percentage of residents without health insurance.
Kentucky’s bottom-ranked indicators, other than worst of all in Covid-19 hospitalizations, were adults who report fair or poor health, adults without a dental visit in the past year, adults who have lost six or more teeth, adults who smoke, children who are overweight or obese (all next to last)) and preventable hospitalizations of seniors (47th, or fourth from the worst).
In the overall ranking of health systems, Kentucky was sixth among the 12 southeastern states (Alabama, Arkansas, Florida, Georgia, Kentucky, Louisiana, Mississippi, North Carolina, South Carolina, Tennessee, Virginia and West Virginia).
Kentucky’s pandemic management and outcomes
The scorecard shows the impact of the pandemic on each of the measured domains; states that entered the pandemic with stronger health status and systems fared better with the pandemic. Hawaii, Maine, Vermont, Washington, and Oregon ranked tops in handling the pandemic, while Alabama, Oklahoma, Kentucky, Mississippi, and Georgia ranked at the bottom.
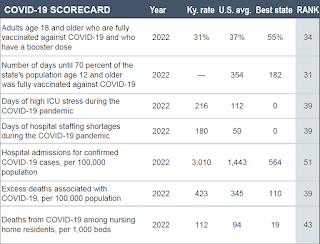 |
| Commonwealth Fund table, adapted by Kentucky Health News |
Among the seven indicators used to measure the Covid-19 response in states and Washington, D.C., Kentucky ranked ninth for Covid-19 deaths among nursing home residents.
And despite a huge effort by state officials to get Kentuckians vaccinated, the state ranked 34th in percentage of fully vaccinated adults who had gotten a booster shot by the end of March 2022 (31%)
Kentucky ranked 39th for three Covid-19 indicators: days of high use of intensive-care units (126 days); days of hospital staffing shortages (180); and excess deaths from February 2020 through March 2022. Excess deaths are the number above what would have been expected from historic mortality patterns; they include Covid-19 deaths.
“Because the pandemic disrupted their ability to get timely care for conditions other than Covid-19, many more people likely died sooner than they otherwise would have,” says the report.
Asked if these rankings have more to do with the strength or weakness of the state’s health-care systems than states’ policies to address the pandemic, Sara Collins, vice-president of coverage and access for The Commonwealth Fund, said it’s important to look at the whole picture to understand why Kentucky has such a low Covid-19 score.
For example, she noted that while Kentucky expanded Medicaid and has a low uninsured rate, it also has high Covid-19 hospitalization rates and a highly vulnerable population that has high levels of pre-existing health conditions like obesity and smoking.
“It just goes to show you that coverage is a necessary condition for access to health care and good outcomes, but it is not a sufficient condition,” she said.
The state Cabinet for Health and Family Services was asked for comment on Kentucky’s ranking of 49th in handling the pandemic, but did not respond before the 12:01 a.m. Thursday time of publication.
Other indicators affected by the pandemic
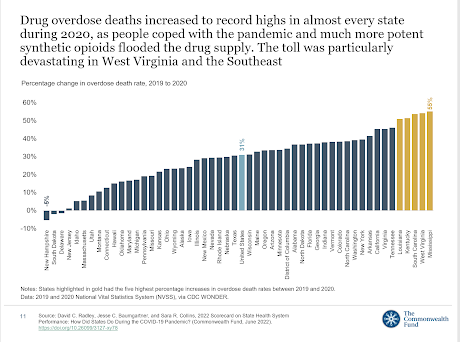
The indicator that worsened most in Kentucky during the pandemic was drug-overdose deaths. Kentucky ranked third for this measure, with 49 overdose deaths per 100,000 residents, a 51% increase from 2019 to 2020.
“Immediately after the pandemic began, deaths spiked, as people dealt with physical isolation, disrupted addiction treatment, and a supply of deadlier drugs like fentanyl,” says the report.