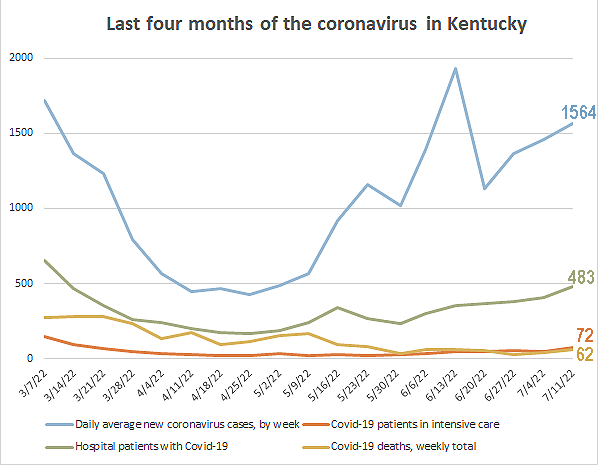
Kentucky Health News graph from state data; for a larger version, click on it.
—–
By Melissa Patrick
Kentucky Health News
All the metrics used to measure the coronavirus in Kentucky went up last week, including new cases, the share of Kentuckians testing positive for the virus, and Covid-19 hospitalizations and deaths.
The share of Kentuckians testing positive continued on a steady rise, increasing to 16.96% from 15.75% in the previous Monday-through-Sunday reporting period. The figures do not include home tests.
The state attributed 62 more deaths to Covid-19 last week, an average of 8.86 per day, a big jump from the previous week’s 38, a rate of 5.43 per day. The state’s pandemic death toll is 16,224.
The state’s report for last week shows 10,949 new coronavirus cases, an average of 1,564 per day. Last week, the daily average of new cases was 1,368. The increase from week to week was 14.3%.
The statewide incidence rate increased to 33.98 cases per 100,000 population, the highest sicne Feb. 25, up from 30.77 in the previous report. The top 10 counties were Rowan, 64.8 per 100,000; Perry, 63.8; Muhlenberg, 57.4; Wolfe, 55.9; Robertson, 54.2; Mercer, 53.4; Bourbon, 51.3; Simpson, 50.8; Lyon, 50.5; and Boyd, 49.5.
The New York Times ranks Kentucky’s case rate 18th among the states, with a 7% drop in cases in the last 14 days.
Covid-19 hospital numbers remain low, but keep ticking up. Kentucky hospitals reported 484 patients with Covid-19, up from 405 a week ago, with 72 in intensive care (up 23) and 28 on mechanical ventilation (up five).
The latest
Centers for Disease Control and Prevention national Covid-19 risk map, which estimates risk through new-case numbers and hospital capacity, shows 37 counties with a high level of coronavirus transmission and 44 with a medium risk. The map is updated on Thursday evenings.
Feds won’t reveal data on spread in hospitals
Politico reported in June that the Biden administration considered publicly releasing data detailing how prevalent Covid-19 spread inside individual hospitals during the Omicron wave, but decided to keep it secret.
Rachel Levy reports, “The decision to withhold the names, based partly on concerns about duplicative data and partly on fears of embarrassing hospitals, denies patients the opportunity to steer clear of health systems with poor track records and allows facilities to avoid public scrutiny, patient advocates say.”
The American Hospital Association wants facilities’ infection numbers to stay private. “Reporting aggregate data is the most appropriate approach given the very low occurrence of hospital onset Covid-19,” Nancy Foster, an AHA executive, said in a statement.
Ginger Dreyer, senior director of communications for the Kentucky Hospital Association, and Susan Dunlap, spokeswoman for the Cabinet for Health and Family Services, both said they did not have any data on hospital-transmitted Covid-19 infections.
Dr. Kevin Kavanagh of Somerset, an infection-control activist and board chairman of
Health Watch USA, writes about this issue in an
op-ed for the Louisville
Courier Journal, calling the design to measure hospital-acquired Covid-19 “severely flawed,” resulting in what he says is likely a big undercount.
“The estimates of the hospital-acquired Covid-19 in the United States are almost assuredly drastic undercounts, but no one knows because no one is truly counting,” he writes, adding that many hospital employees don’t feel safe, “worsening the chronic nursing staff shortage. The CDC must set the highest standards for the world to emulate, not standards that are pliable for our profit-driven health care systems.”
The state’s latest report shows five of Kentucky’s 10 hospital regions are using at least 80% of their intensive-care beds, with Northern Kentucky having the highest percentage of Covid-19 patients in them, 7%. Eastern Kentucky is only at 59.55% ICU capacity, but 8.6% of its ICU patients have Covid-19.
