Everyone 45 and older should be screened for colon cancer, earlier if you have a family history of it; Kentucky has made much progress on this front
Kentucky Health News
March is Colorectal Cancer Awareness Month, which serves to remind everyone who is 45 and older – or is younger than 45 with a family history of colon cancer – to get screened.
That’s because colorectal cancer is one of the leading causes of cancer-related deaths in Kentucky and often doesn’t cause any symptoms, especially in early stages when the only way to detect it is through screening, says Dr. Avinash Bhakta, a colorectal surgeon at the University of Kentucky Markey Cancer Center.
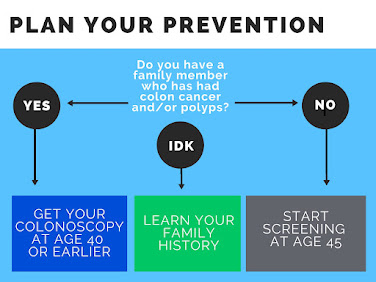
The Colon Cancer Prevention Project says regular screening is recommended to strat at 45 for people who do not have a family member who has had colon cancer and/or polyps. Those who have a family history of colon cancer should get a colonoscopy at age 40 or earlier.
UK’s Bhakta writes that while colonoscopy is the gold standard for screening that must be done in a clinic or hospital under sedation, stool-based tests offer an alternative that is less invasive and can be more accessible.
“Twenty years ago, Kentucky had the highest colorectal cancer incidence and mortality rates in the U.S., as well as the second-lowest colorectal cancer screening rate,” Elizabeth Chapin reports for UK. “Today, thanks to the coordinated efforts of state agencies and organizations, these dire statistics have turned around. Since 2002, colorectal cancer screenings have doubled in Kentucky, which has led to a more than 30% decrease in incidence and mortality rates.”
Much of this success is due to efforts made by the Kentucky Cancer Consortium in collaboration with several major cancer groups that worked to make colorectal screenings more accessible to Kentuckians.
“What we’ve seen happen with colorectal cancer rates in Kentucky over the past two decades is truly a public health success story,” Thomas Tucker, the Markey Cancer Center’s senior director for cancer surveillance, told Chapin. “It goes to show that significant change can happen when we work together and coordinate our efforts.”
“The results have saved thousands of lives,” Tucker told Chapin. “To put it into perspective, today, 650 fewer Kentuckians are diagnosed and 270 fewer die from colorectal cancer each year than in 2001.”
Despite Kentucky’s progress, Chapin reports that roughly a third of eligible Kentuckians still do not seek colorectal cancer screenings due to health, socioeconomic and education disparities.