Most people have end-of-life wishes, but don’t talk about it; planning for death is less likely in rural areas, study finds
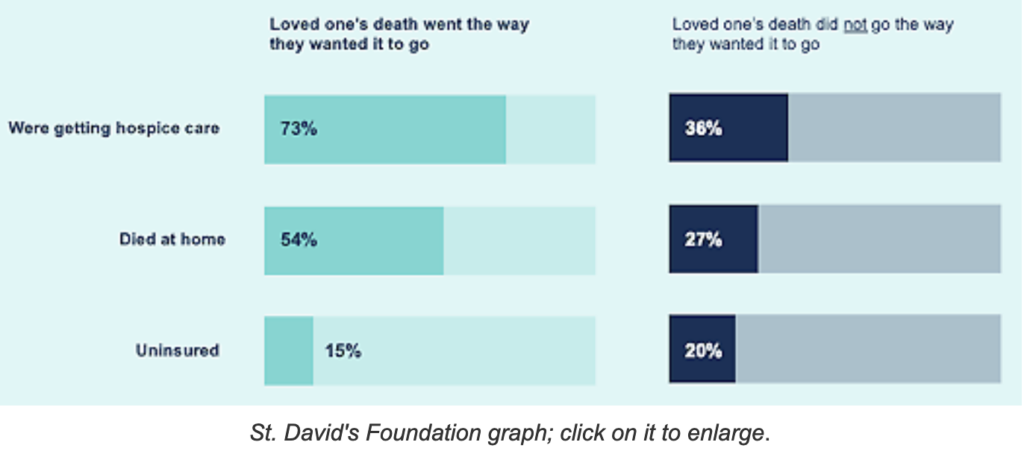
Researchers from St. David’s Foundation in Texas found that when it comes to end-of-life care, most Texans want to die at home (76%) and not be a burden to their families (77%). “But only one in three people surveyed said their loved one’s wishes were honored,” Carey writes. “Of those who are least likely to have their end-of-life wishes followed are rural residents, the study found. . . . Only 37% of the survey respondents said their loved ones died at home. Close to half of them (47%) said their loved one faced challenges related to their care – from problems with insurance coverage to facing cultural or language barriers.”
Honoring a person’s wishes begins with knowing what they are. Andrew Levack, senior program officer with St. David’s Foundation, told Carey: “One of the interesting things the study found was how few conversations respondents had with their doctors around plans for end of life. I think people have an idea of what they would like, but it takes some active planning and advocacy to make that happen.”
Study researchers noted a common thread of disconnection across the state — people have end-of-life care desires, but don’t voice them. “Most Texans, even older adults, are unprepared for decisions about end-of-life care. The vast majority believe it is important to have their wishes in writing, yet over half have not done so. Similarly, many say they would like to discuss end-of-life planning with their health care provider if they were faced with a serious illness, yet only 17% have had a provider initiate a conversation about it.”
Geographical isolation and a lack of health care access make rural populations more likely to not have end-of-life plans or discussions. Dr. Kate Tindell, medical director for Austin Palliative Care and Hospice, told Carey: “People have really disjointed health care now. We’ve sort of lost that sense that there is a captain of the medical ship who is aware of all the moving parts and is giving the patient that guidance. I think that really causes people to not have the kind of relationship that would allow them to have that kind of conversation (about end-of-life wishes) the way they would if they had seen the same provider every single time for 10 years.”