Health-care forum examines ‘incredible change’ in Kentucky’s health-care system, looks forward to more access to care
Kentucky Health News
What does health-care reform mean to Kentucky? What impact has Medicaid expansion had? Can we work together to do care differently in Kentucky? Answers to these questions and more were offerd by national, regional, and local health care experts Sept. 16 in Louisville at the Foundation for a Healthy Kentucky‘s annual Howard L. Bost Health Policy Forum.
This year’s topic was “Doing Care Differently,” but as foundation chair David Bolt, deputy director of the Kentucky Primary Care Association, told the crowd, “It could have just as easily been named after the Bob Dylan song, ‘The Times They Are A-Changin’.”
As a health-care provider for 44 years, Bolt said, “I have lived through almost every change since the implementation of Medicare and Medicaid. And I am actually excited about the changes I see on the horizon.” He said he thinks the late Dr. Bost would look at what Kentucky is doing and say,” It’s about time we moved away from a treat-’em-and-street-’em mentality to integrated health care delivery services and systems rooted in accountable outcomes and founded in a value-drive system of improving health.”
One of the biggest recent changes in Kentucky health care is Gov. Steve Beshear’s expansion Medicaid at the beginning of the year, which offered coverage to Kentuckians under 65 in households up to 138 percent of the federal poverty level. As a result, Medicaid is now the largest health-care payer in the state, serving 1.1 million Kentuckians, one out of every four, Cabinet for Health and Family Services Deputy Secretary Eric Friedlander told the crowd.
“We had incredible enrollment. It’s an incredible change.” said Friedlander. “We hope it is a change for the better.”
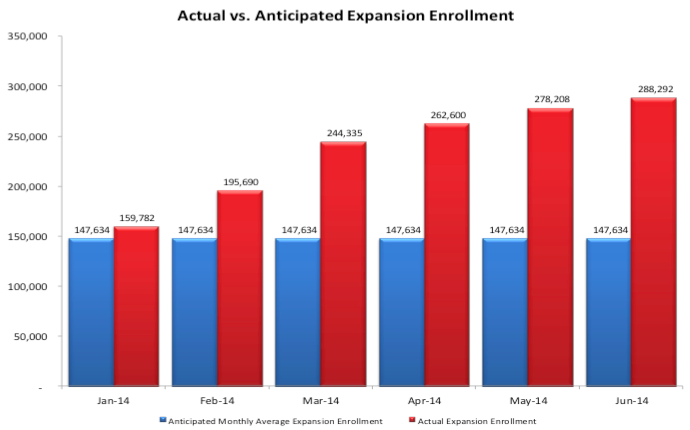
Friedlander said enrollment in every county exceede estimates for the state by the accounting firm PriceWaterhouse Coopers, based on estimates from the Congressional Budget Office. Those estimates anticipated 55 percent of eligible persons enrolling in the first year, leveling out at 70 percent in future years. Instead, enrollments through June were almost double the prediction.
Medicaid paid more than $284 million to Kentucky health-care providers in the first half of this year for treating the newly eligible Medicaid beneficiaries, with hospitals receiving 48 percent of those reimbursements, Friedlander said. He said that number will be $1 billion to $2 billion by the end of the year. (Medicaid payments sometimes take months to complete.)
The federal government is paying the entire cost of the newly eligibles through 2016. State officials have said that they won’t be able to update cost estimates for 2017 a few more months because additional data must be collected about enrollees after the insured population has stabilized.
“Medicaid expansion is not static,” Friedlander said. “It is dynamic, and the individuals that make up that enrollment are constantly changing.”
Friedlander said employment in Kentucky health care has increased by 3,800 jobs, but the study estimated that 7,600 jobs would be added in the first year. This means enrollment is almost double what was projected yet job expansion is almost half. That undercuts Beshear’s contention, based on the study, that Medicaid expansion will pay for itself by adding heath-care jobs.
As more Kentuckians get insurance, there may be shortages of primary-care doctors, especially in rural areas of states like Kentucky, reports Kaiser Health News. That need could be overstated, Sheila Schuster, a clinical psychologist and executive director of the Advocacy Action Network, said at the forum.
Kentucky has 3,929 advanced practice registered nurses, Schuster said, 54 percent more APRNs than in 2010. A new state law that took effect July 15 “removed a barrier that was keeping them from opening practices,” she said. The law allows APRNs to prescribe non-narcotic drugs independently after they have prescribed under physician supervision for four years.
The law was passed after negotiations among the Kentucky Medical Association, the Kentucky Academy of Family Physicians and the Kentucky Coalition of Nurse Practitioners and Nurse Midwives. Schuster suggested that other such compromises are needed to expand access to health care.
“We aren’t playing very well with each other in the sandbox,” she said, adding that turf battles need to be set aside to keep health-care innovation people-centered.
The forum was co-sponsored by KET, Louisville’s Health Enterprises Network, the Kentucky Health Information Exchange, the Kentucky Medical Association and Leadership Kentucky.
